
The Debate Is Over: Antidepressants DO Work Better Than Placebo
The idea that antidepressants are no more effective than placebo has been put to rest. They clearly work when used appropriately, although the effect size is not as large as the published studies have suggested.

Texas: Ground zero for the politicization of school vaccine mandates
Vaccine policies and school vaccine mandates have traditionally been as close to a nonpartisan issue as there can be in the US. Unfortunately, in Texas antivaccine activists and conservative activists threaten to change that. The antivaccine group Texans for Vaccine Choice has formed an unholy alliance with antiregulation conservative activists to attack school vaccine mandates. Antivaxers all over the country are doing...

Congress can easily end Medicare waste, fraud and abuse by chiropractors, saving billions
Yet another government report finds chiropractors are bilking Medicare billions for unnecessary services. A simple amendment to the Medicare law could end this, but will Congress act?

Chiropractor Lost His License; Patient Lost Her Uterus
Practicing after he lost his license, chiropractor Nicholas LeRoy used escharotics to treat a woman's cervical dysplasia. As result, she lost her uterus. Ex-naturopath Britt Hermes was taught to use escharotic treatments at Bastyr; she has since realized that they are "unproven, dangerous, and very stupid."
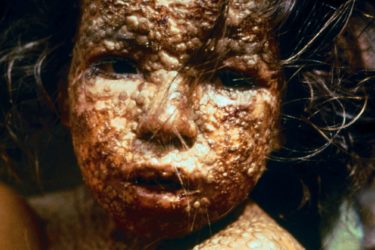
The So-Called Vaccine Debate: False Balance in The San Diego Union-Tribune
A recent article in The San Diego Union-Tribune presents a pair of articles that gives a false balance regarding vaccinations. Those who oppose vaccination do so on the basis of ideology rather than science, thus placing the public's health at risk.

The Six Month Dental Recall – Science or Legend?
The evidence to support dental cleaning every six months is...less than ideal, but it still may be a good idea for many people.

Are we all contaminated with chemical toxins?
Are we all being gradually poisoned by environmental toxins? And what is the evidence for detoxification kits and cleanses?
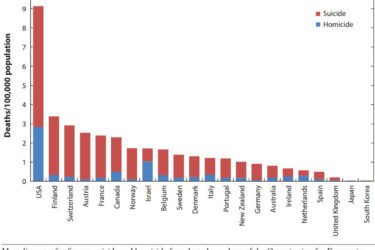
Gun Violence as a Public Health Issue
Gun violence is a serious public health issue in America but is not getting the research that it deserves. This needs to change.

A Cornucopia of Crislip
Mark Crislip has written three books. They are full of wisdom, science-based thinking, and hilarious humor. Highly recommended.





Where Are We With the Replication “Crisis”
The replication problem is not as bad as the sensational reporting has suggested. But it is still a legitimate issue that needs to be addressed.