
Are we all contaminated with chemical toxins?
Are we all being gradually poisoned by environmental toxins? And what is the evidence for detoxification kits and cleanses?
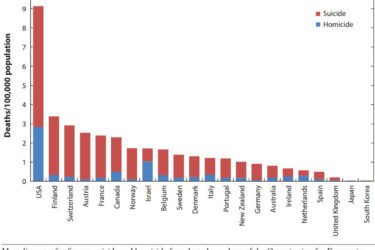
Gun Violence as a Public Health Issue
Gun violence is a serious public health issue in America but is not getting the research that it deserves. This needs to change.

A Cornucopia of Crislip
Mark Crislip has written three books. They are full of wisdom, science-based thinking, and hilarious humor. Highly recommended.

True believers, entrepreneurs, and scammers in alternative medicine
In the online echo chamber promoting alternative medicine, there are varying degrees of deception. There are true believers (who are often victims), entrepreneurs (who are often true believers who found a profitable business), and scammers. The categories are not mutually exclusive.

Inside Chiropractic: Yesteryear and Today
In the 123 years since its inception, the core beliefs of the chiropractic profession have not changed. Chiropractic continues to exist as a form of alternative medicine that embraces a variety of questionable procedures and treatment methods. The chiropractic profession in the United States is still defined by the vertebral subluxation theory that gave it birth and independence as an alternative to...

Cleveland Clinic genetic experts call out functional medicine on worthless genetic testing and supplement prescribing
Cleveland Clinic genetics experts call out functional medicine on worthless genetic testing and dietary supplement prescribing: "Poor science, leading to even worse medicine." Irony meters exploded everywhere.

Move
For most people, common health goals are best approached with as simple a strategy as possible. This avoids cognitive overload and non-compliance. Get the basics right, as there are diminishing returns from increasingly arcane details.

Quackademic medicine and the delusion of being “science-based”
Last week, I was interviewed by the a reporter from the Georgetown student newsletter about its integrative medicine program. It got me to thinking how delusion that one's work is science-based can lead to collaborations with New Age "quantum" mystics like Deepak Chopra.

The 2018 Flu Epidemic: Hives and other Influenza Related Nonsense
While it isn't likely to be the flumaggedon, it is shaping up to be a really bad flu season. Unfortunately there is a lot of overzealous news coverage that I fear is causing more anxiety among parents than is warranted.






Answering Our Critics – Again!
Critics of Science-Based Medicine keep making the same old tired arguments, despite the fact that their arguments have been repeatedly demolished. Here is a list of recurrent memes, with counterarguments.