Is the use of “Open-Label” Placebo Ethical in the Treatment of Children?
Is the use of "open-label" placebo ethical in pediatric medical care, or any care for that matter? A recent article in Pediatrics discussing this issue comes to a flawed conclusion based on a misunderstanding of placebo and of the literature on placebo without deception.

Statins beat supplements
Red yeast rice supplements have poor quality control and there's no clear evidence they do anything beneficial. So why take it?
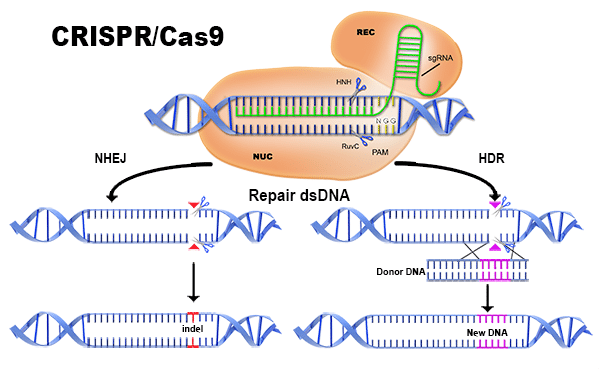
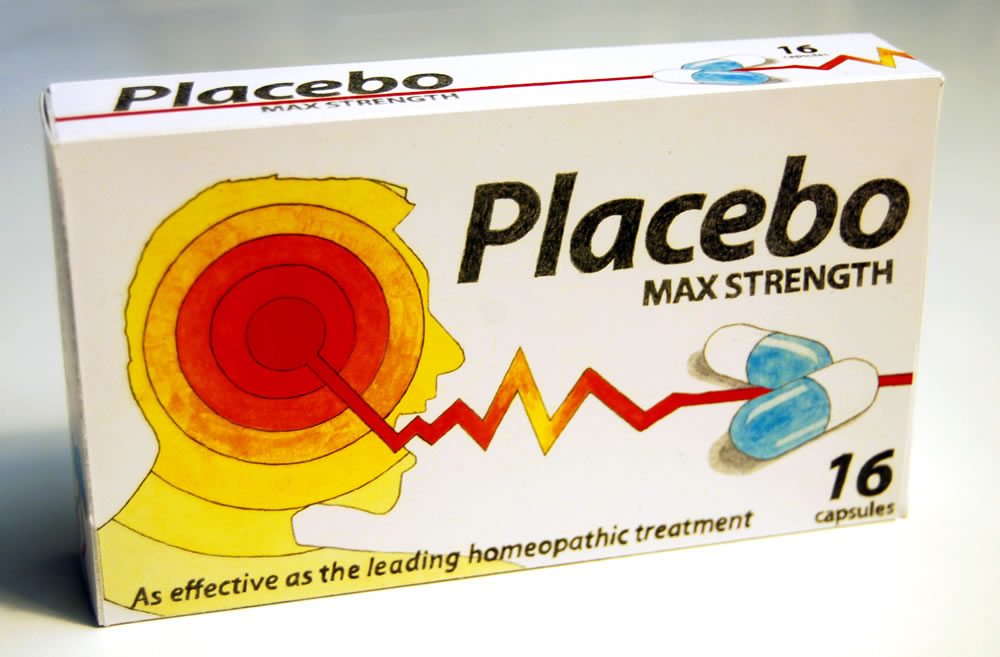
The Promise of CRISPR
CRISPR is the latest rock-star medical technology that promises to revolutionize medicine. Let's take a look at the hype and the reality.

Viotren and Other Dietary Supplements for Erectile Dysfunction: Buyer Beware
Viotren and other dietary supplements are being illegally marketed to treat erectile dysfunction. Some of them work, but only because they are adulterated with prescription drugs like Viagra (at up to 31 times the prescription dose). Using them can be risky.

No, a Vaccine Court ruling does not show that vaccines cause SIDS
There was a rumbling in the antivaccine underground over the weekend about a recent ruling by the Vaccine Court compensating parents of a child who died of sudden infant death syndrome (SIDS). In a confused and scientifically highly flawed decision, the Special Master Thomas Gowen didn't rule that vaccines cause SIDS, but did rule that they contributed to SIDS in this one...

The Congressional Dietary Supplement Caucus
The Congressional Dietary Supplement Caucus, an officially-recognized Congressional Membership Organization, operates as an in-house mouthpiece for the dietary supplement industry. Both the caucus and the rules allowing it should be reformed to prohibit this.

The Supplement Con
A new article in Business Insider challenges the major narrative promoted by the supplement industry - that supplements are safe, effective, natural, and actually in the bottle. If we are lucky, this may mark a the start of a sea change in how Americans see supplements.

The Hormone Myth
"Mary is really bitchy today; she must be on the rag." Comments like this are all too common, and are misguided. In her new book, Robyn Stein DeLuca dispels the myths about how hormones affect women's moods and mental health, myths that have contributed to unequal treatment of women. Junk science supported the myths; good science debunks them.
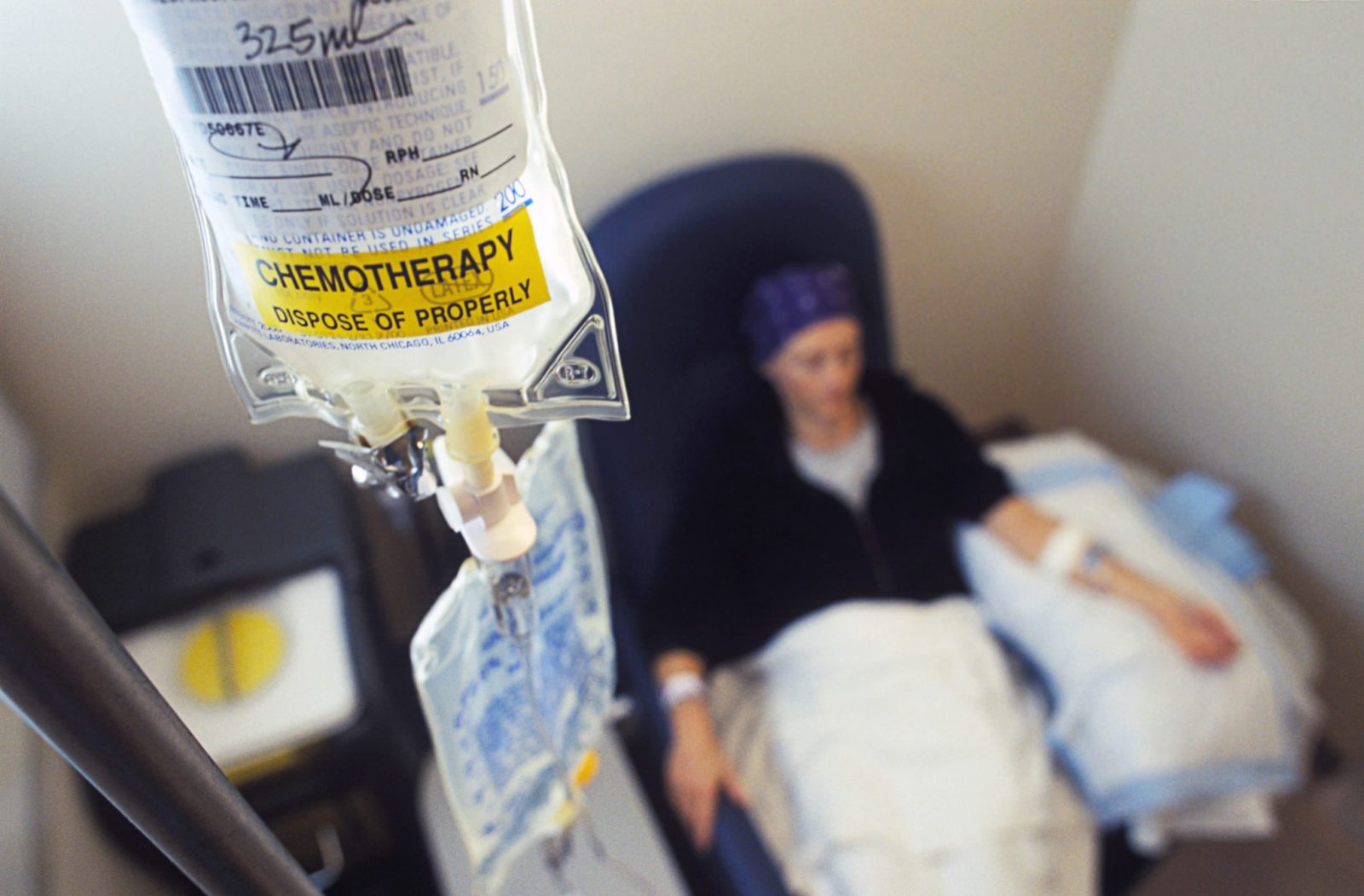
Alternative medicine kills cancer patients
By definition, alternative medicine has not been shown to be effective or has been shown to be ineffective. Thus, alternative medicine is ineffective against cancer and can best be represented as either no treatment at all or potentially harmful treatment. It is thus not surprising that cancer patients who choose alternative medicine have a higher risk of dying from their cancer. A...