
Naturopathic conquest of New England nears completion
Rhode Island is poised to become the latest state to succumb to the false notion that licensing naturopathic “doctors” will protect the public health and safety, making naturopathic conquest of New England complete.

New Review of Artificial Sweeteners
A new review of research finds a modest but inconsistent benefit from consuming artificial sweeteners over sugar. Their conclusion of a possible backfire effect, however, does not seem to be supported by the studies they review.

Most Patients Get No Benefit from Most Drugs
Some people are reluctant to take statins because they don't benefit the majority of patients who take them. Actually, most drugs don't benefit most of the patients who take them. Since we have no way of identifying those who will benefit, we are stuck treating the many to benefit the few.

Sen. Ron Johnson: Holding the bill funding the FDA hostage unless the cruel sham that is right-to-try is added to it
Advocates claim that "right-to-try" laws help terminally patients by allowing them access to experimental drugs before approval, when, in fact, such laws strip legal and regulatory protections from patients using such drugs and their purpose is actually to undermine and weaken the FDA. Now advocates led by Sen. Ron Johnson (R-WI) are making a new push to pass right-to-try by embedding it...
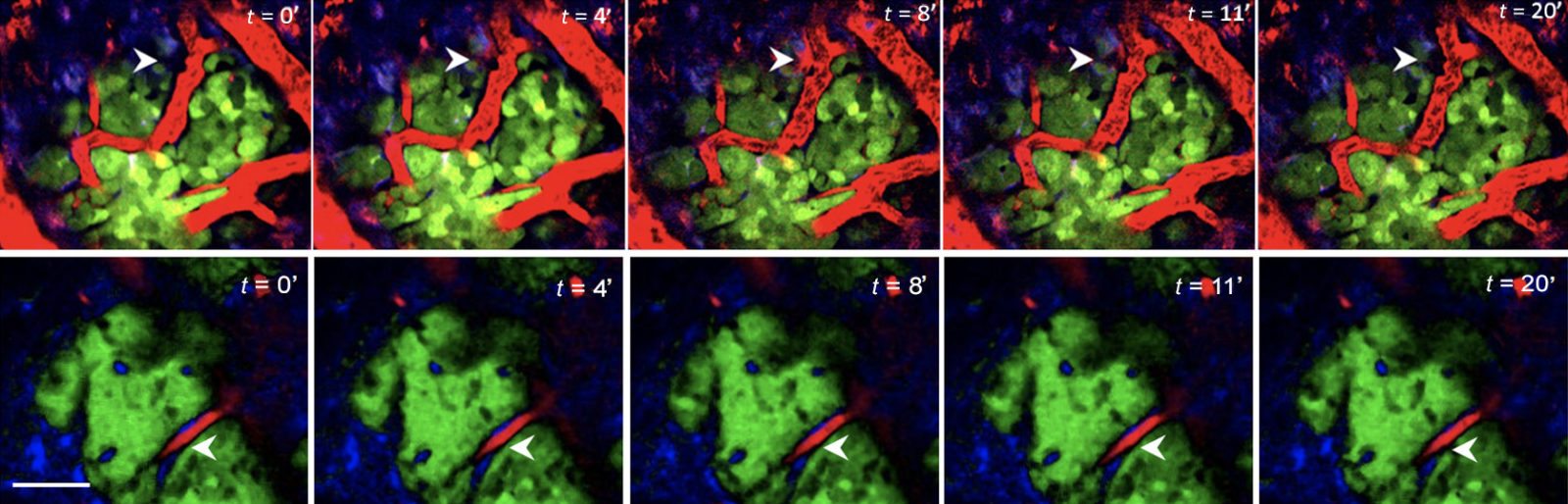
Does chemotherapy cause cancer to spread?
Earlier this month, a study was published in Science Translational Medicine that showed how chemotherapy before surgery can stimulate breast cancer invasiveness and invasion under certain circumstances. Not surprisingly, alternative cancer cure mavens everywhere are spinning the study as "proof" that chemotherapy has no benefit and causes only harm (and so you should buy their nostrums instead). Unsurprisingly, the actual results are...

Placentophagy and the Risk of Invasive Neonatal GBS Disease
A young infant has suffered an invasive and potentially deadly bacterial infection...twice! Now the CDC is warning that maternal placentophagy may have played a role.
Australian review: Get homeopathy out of pharmacies
An independent review of Australian pharmacy practice has recommended that homeopathic products be kept out of pharmacies.
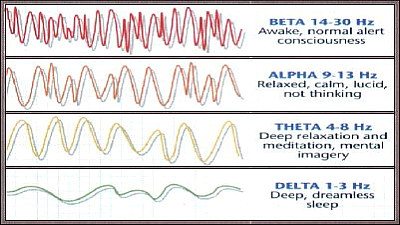
Brain Wave Pseudoscience
iSynchrony has put together a plausible-sounding bit of bafflegab to justify what it sells. The reality of neurology is against their claims.

What the Health: A Movie with an Agenda
The documentary "What the Health" espouses the fairy tale that all major diseases (heart disease, diabetes, cancer, and many others) can be prevented and cured by eliminating meat and dairy from the diet. It is a blatant polemic for veganism, biased and misleading, and is not a reliable source of scientific information.

Trump’s new CDC Director is very pro-vaccine, but was she also at one time a quack?
On Friday, Health and Human Services Secretary Dr. Tom Price announced the appointment of Dr. Brenda Fitzgerald to head the CDC. Reassuringly, her record as Georgia Public Health Commissioner was pro-vaccine and relatively non-ideological. Not so reassuringly, a news report yesterday found that before entering public service she was peddling anti-aging quackery at her private practice. Where will her balance fall now...






Don’t Blame the Patient