Category: Acupuncture

The Beekeeper: Sentinel Chicken?
Bee venom. Will it help Andy's rheumatism? Doubtful
Medicare and Alternative Medicine
Medicare is paying for nonsense.
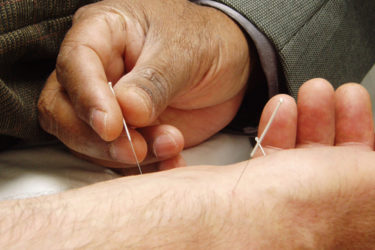
Aromatase inhibitors and acupuncture in breast cancer: Spinning a negative study, four years later
Four years ago, I wrote about an essentially negative study looking at whether acupuncture could alleviate joint pain caused by aromatase inhibitors, a common treatment for estrogen-sensitive breast cancer. The study's back, and it doesn't look any more positive.

Some Sepsis Stuff
Sepsis interventions. Some don't work and some don't work.

Alternative Reproduction?
Are there effective forms of SCAMs for birth control or reproduction? Of course not.

Zeno’s Paradox
An elderly German experiments with a new form of acupuncture. Time says acupuncture is entering the mainstream. Acupuncture has been trying to enter for decades. Still not close.
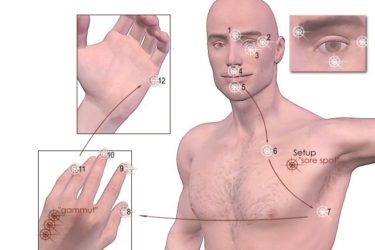
Emotional Freedom Technique – Acupuncture for the Mind
Emotional Freedom Technique is based in pseudoscience and inadequate clinical research.

Science-based medicine isn’t just for CAM. The case of ivermectin shows that it never was.
Another large randomized controlled trial for ivermectin showed no efficacy for the early treatment of COVID-19. This is not a surprise to science-based medicine advocates. Here's why the story of ivermectin shows that SBM isn't just for "complementary and alternative medicine" (CAM) —and never was.

Allergy Release Technique
A dubious intervention for food allergies follows a typical pattern for such treatments.


