Science-Based Politics: Lyme, Zika, and the Green Party.
I don’t have much to write about this week. Yeah, yeah, I know. How is that different than the last 50 blog entries? And I will have even less to say next time. But nothing of real interest has crossed my screen the past two weeks, not that I have really been looking. One of my favorite stories as a kid was...
Kratom: another dangerous “natural” remedy
Kratom (Mitragyna speciose) is a tropical tree from Southeast Asia whose leaves are traditionally chewed or prepared as a powder. Native populations chew the leaves to reduce fatigue when doing manual labor, such as working on rubber plantations. It is also used in cultural performances and consumed as a drink prepared from kratom powder. When the Second World War caused an increase...
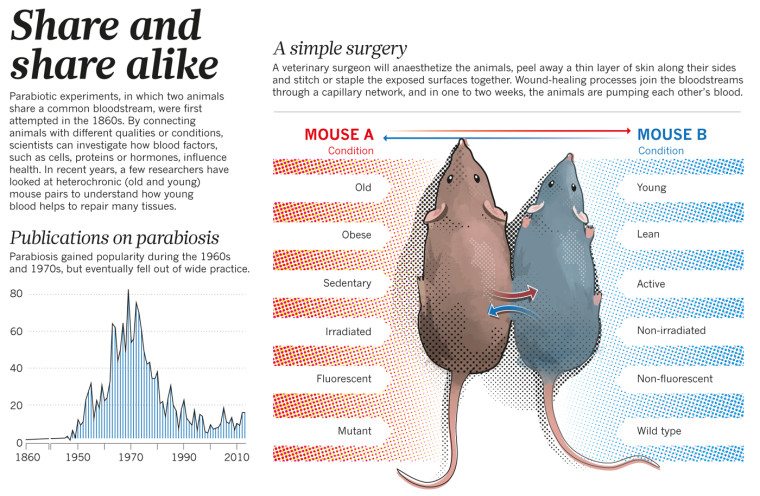
Parabiosis – The Next Snakeoil
The pattern has repeated so many times that it is truly predictable. Scientists turn their eyes to one type of treatment that has theoretical potential. However, proper research from theory to proven treatment can take 10-20 years, if all goes well. Most such treatments will not work out – they will fail somewhere along the way from the petri dish to the...

Statistics Done Wrong, And How To Do Better
Statistics is hard, often counterintuitive, and burdened with esoteric mathematical equations. Statistics classes can be boring and demanding; students might be tempted to call it “Sadistics.” Good statistics are essential to good research; unfortunately many scientists and even some statisticians are doing statistics wrong. Statistician Alex Reinhart has written a helpful book, Statistics Done Wrong: The Woefully Complete Guide, that every researcher...

Dealing with vaccine hesitancy and refusal
Almost as long as there have been vaccines, there has been an antivaccine movement. The misinformation promoted by antivaccinationists can infect parents and make them vaccine-averse. Here, we deal with some antivaccine tropes that find their way to the vaccine-averse.
Separating Fact from Fiction in Pediatric Medicine: Facial Nerve Palsy
There are numerous medical conditions that are seemingly designed to allow proponents of “irregular medicine” to proclaim their treatments to be effective. These conditions tend to be chronic and subjective in nature, or to have waxing and waning courses such that a parent or patient might easily be fooled into assigning a causal relationship between a bogus intervention and a clinical improvement....
CARA: Integrating even more pseudoscience into veterans’ healthcare
The pixels were barely dry on David Gorski’s lament over the expansive integration of pseudoscience into the care of veterans when President Obama signed legislation that will exacerbate this very problem. The “Comprehensive Addiction and Recovery Act of 2016” (“CARA”) contains provisions that will undoubtedly keep Tracy Gaudet, MD, and her merry band of integrative medicine aficionados at the VA busy for...
Past Life Regression Therapy: Encouraging Fantasy
I recently got an e-mail from a PR firm about an “internationally certified regression therapist,” Ann Barham, who has written a book and who claims to help patients to “heal enduring challenges, release unhealthy patterns and beliefs, and find their way to more happiness and success.” They offered me the opportunity to review her book and/or interview her; I declined, but I...






The Public’s Love-Hate Relationship with Technology
There are many complex factors driving up the cost of healthcare, but one major factor is increasing medical technology. Often new expensive technologies provide incremental, or even questionable, additional benefits but can dramatically increase the cost of health care. This is especially true of in-hospital treatments. There are also, of course, medical technologies that provide significant benefits, and others that improve our...