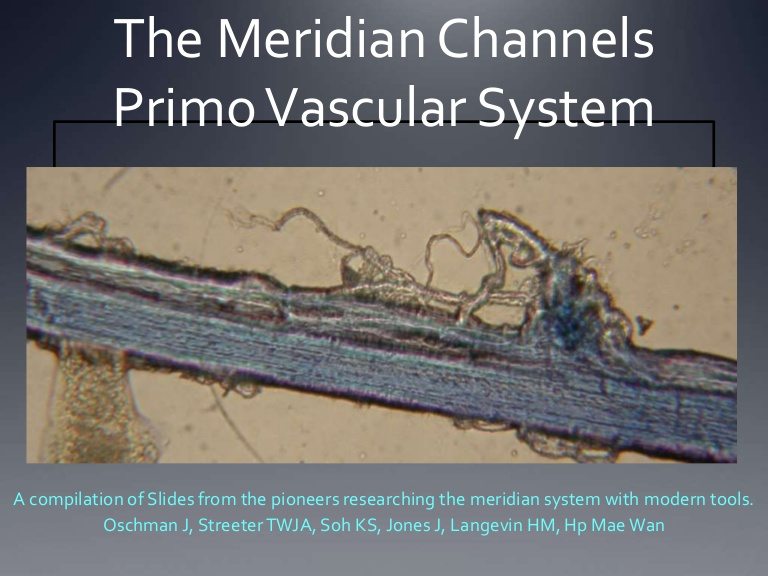
The Primo Vascular System: The N-rays of Acupuncture?
Acupuncture meridians and acupoints are imaginary until proven otherwise. Anatomists have never been able to detect them by microscopy or autopsy, and they are not mentioned in anatomy textbooks. For decades, acupuncturists have been trying to prove that their pre-scientific belief system is grounded in scientific reality. Now they are telling us that acupuncture meridians and acupoints have been discovered in the...

Is there a reproducibility “crisis” in biomedical science? No, but there is a reproducibility problem
Reproducibility is the key to scientific advancement. It has been claimed that we suffer from a "reproducibility crisis," but in reality it is a chronic problem in reproducibility. Here we will look at the scope of the problem and strategies to address it.
False balance about Stanislaw Burzynski and his disproven cancer therapy, courtesy of STAT News
One common theme that has been revisited time and time again on this blog since its very founding is the problem of how science and medicine are reported. For example, back when I first started blogging, years before I joined Science-Based Medicine in 2008, one thing that used to drive me absolutely nuts was the tendency of the press to include in...
Does your antivax doctor have another agenda?
Several weeks back, I wrote a piece in praise of Michigan’s Fresh Air Camp’s decision to admit only properly vaccinated children. Predictably, there was a bit of a backlash from people who, despite the obvious benefits, oppose vaccinations. I can’t fault a parent for the decisions they make for their kids. We all work from the gut when it comes to our...
Newborn Phototherapy and Cancer: Cutting Edge Research or “Big Data” Failure?
While social media and news outlets were reacting, or in some cases overreacting, to a new rodent-based medical study on the unlikely link between cell phone use and brain cancer last month, two studies and an accompanying commentary were quietly published in Pediatrics that raised similar concerns. Rather than cell phone use, the proposed potential cause of pediatric cancer in these newly...
Fooling Myself
The first principle is that you must not fool yourself — and you are the easiest person to fool. –Richard Feynman I like to think of myself as a rational person, but I’ve been fooled by my own experience again and again. I’ve made bad decisions and wasted time and money believing what I was seeing, instead of being objective and looking...
PET Scans Predict Coma Outcome
A new study shows that 42 really is the answer to life, the universe, and everything. OK, not really, but it does show that 42% of healthy brain activity is the minimum threshold for consciousness. Disorders of consciousness, also referred to as coma when severe enough, can be a difficult situation to assess sufficiently to make reliable predictions about outcome. Part of...
Therapeutic Touch Pseudoscience: The Tooth Fairy Strikes Again
A study out of Iran titled “Therapeutic touch for nausea in breast cancer patients receiving chemotherapy: Composing a treatment” was recently published in the journal Complementary Therapies in Clinical Practice. It is a great example of the Tooth Fairy science that permeates much of the research in complementary and alternative medicine. In Tooth Fairy science, researchers attempt to study a phenomenon without...
No, a rat study with marginal results does not prove that cell phones cause cancer, no matter what Mother Jones and Consumer Reports say
There are certain myths that are frustratingly resistant to evidence, science, and reason. Some of these are basically medical conspiracy theories, where someone (industry and/or big pharma and/or physicians and/or the government) has slam-dunk evidence for harm but conspires to keep it from you, the people. For example, despite decades worth of negative studies, the belief that vaccines are harmful, causing conditions...
Dry Needling
War, huh, yeah What is it good for Absolutely nothing Uh-huh huh War, huh, yeah What is it good for Absolutely nothing Say it again, y’all War, huh, What is it good for Absolutely nothing Listen to me Ohhh, war, I despise Cause it means destruction Of innocent lives War means tears To thousands of mothers eyes When their sons go to...






Don’t Blame the Patient