Tag: antibiotics
Deciding Which Risks to Take
No medical treatment is risk-free. Paul Offit's new book covers the history of innovations that went awry and advises how to balance the risks of new medical innovations with the risk of not treating.
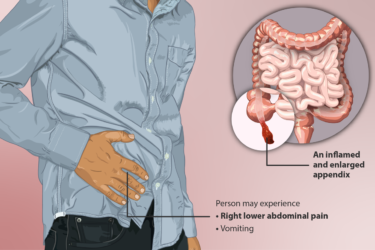
Appendicitis: Surgical vs. Medical Treatment
Surgery or antibiotics for appendicitis? This new study can help with the decision.
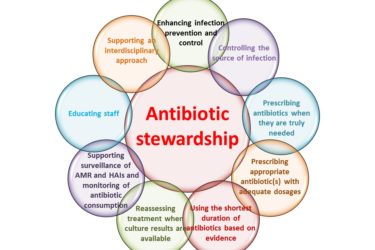
Inappropriate Antibiotic Use is Rampant in U.S. Pediatric Hospitals
A recent study looked at antibiotic use in thousands of hospitalized children and the results weren't great. Too many kids are receiving suboptimal antibiotic prescriptions. One potential solution is an increased focus on, and improved resources for, antibiotic stewardship programs.

More Political Science: Proposed laws protect “Lyme literate” doctors from discipline
"Lyme literate" doctors are scamming patients out of thousands of dollars with needless long-term antibiotics based on a fake diagnosis of "chronic Lyme." So why are state legislators trying to protect these doctors from discipline and make insurers pay for unnecessary treatments?

If you feel better, should you stop taking your antibiotics?
A recent paper suggests that patients would be better off stopping antibiotics when they feel better, instead of completing the entire amount prescribed. Could this approach reduce antibiotic overuse and the risk of widespread resistance?
Antibiotic Prophylaxis For Dental Procedures
Transient bacteremia (bacteria in the bloodstream) is common after dental procedures, but it rarely causes a problem. So, who needs antibiotic prophylaxis before a dental procedure? What procedures? What does the science say?
A closer look at penicillin allergies
While many people believe they may be allergic to penicillin, few actually are. The consequences may be serious.
Overprescribing Antibiotics
Recently I had a cutaneous abscess which was treated (quite painfully) with incision and drainage. My doctor told me that antibiotics were not strictly necessary, but I could have them if I wanted. The idea of any treatment that could resolve the abscess more quickly was appealing, but I did not want to contribute to the unnecessary use of antibiotics so I...
Why Antibiotic Use Scares Me
Editor’s note: Today we present a guest post from fourth-year medical student Joshua Horton, about the looming problem of antibiotic resistance. Welcome! I read a study recently that alarmed me: acute bronchitis is a condition that rarely requires antibiotics, but three quarters of patients presenting with this condition receive a prescription for antibiotics. Even more worrisome, this statistic has not changed in...
Hospitals Slow to Adopt Pediatric Pneumonia Guidelines
While it is both easy and fun to point out the inadequacies of unscientific modalities such as chiropractic and homeopathy, our goal at Science-Based Medicine is the application of a single standard to all medical practice, even if it stings a bit. We are far from perfect. While I firmly believe that most conventional healthcare professionals are good people who strive to...

