Tag: Asthma

Corrigendum. The Week in Review for 05/28/2017.
More measles in Minnesota. Yet another form of acupuncture: Snafu. CAM cancer studies are of poor quality. The future of CAM is LSD.
Corrigendum. The Week in Review for 05/07/2017.
Death from alternative medicine impersonators. An acupuncture study done so acupuncturists can get insurance money? A chiropractor has to refund the feds one million dollars. And more.
Fake treatments for real diseases: A review of allergy and asthma advertisements by naturopaths, chiropractors, homeopaths and acupuncturists
A majority of Canadian chiropractic, naturopathic, homeopathic and acupuncture clinics claim that they can diagnose or treat allergies, sensitivities and asthma.
Should the FDA crack down on homeopathic “remedies”?
In the category of potentially dangerous complementary or alternative medicine, I can think of few products worse than ones claimed to relieve asthma, yet don’t actually contain any medicine. Yet these products exist and are widely sold. Just over a year ago I described what might be the most irresponsible homeopathic treatment ever: A homeopathic asthma spray. If there was ever a...

Dummy Medicine, Dummy Doctors, and a Dummy Degree, Part 2.1: Harvard Medical School and the Curious Case of Ted Kaptchuk, OMD (cont.)
Rave Reviews In 1983, Ted Kaptchuk, the senior author of the recent “albuterol vs. placebo” article, and soon to become the long-time Second-in-Command of the Harvard Medical School “CAM” program, published The Web that Has No Weaver: The book received rave reviews: A major advance toward the synthesis of Western and Eastern theory. It will stimulate all practitioners to expand their understanding...
Dummy Medicine, Dummy Doctors, and a Dummy Degree, Part 2.0: Harvard Medical School and the Curious Case of Ted Kaptchuk, OMD
Review The recent albuterol vs. placebo trial reported in the New England Journal of Medicine (NEJM) found that experimental subjects with asthma experienced substantial, measured improvements in lung function after inhaling albuterol, but not after inhaling placebo, undergoing sham acupuncture, or “no treatment.” It also found that the same subjects reported having felt substantially improved after either albuterol or each of the...
Revisiting Daniel Moerman and “placebo effects”
About three weeks ago, ironically enough, right around the time of TAM 9, the New England Journal of Medicine (NEJM) inadvertently provided us in the form of a new study on asthma and placebo effects not only material for our discussion panel on placebo effects but material for multiple posts, including one by me, one by Kimball Atwood, and one by Peter...

CAM: The Beer Goggles of Medicine
It is summer, the kids are off, and time to write dwindles in the face of sun and golf. Nonsense knows no season, and in my readings this week I came across the phrase “the undeniable power of the placebo.” I will do my best to deny that power at least three times before I crow my conclusion. One of my first...
Dummy Medicines, Dummy Doctors, and a Dummy Degree, Part 1: a Curious Editorial Choice for the New England Journal of Medicine
Background This post concerns the recent article in the New England Journal of Medicine (NEJM) titled “Active Albuterol or Placebo, Sham Acupuncture, or No Intervention in Asthma.” It was ably reviewed by Dr. Gorski on Monday, so I will merely summarize its findings: of the three interventions used—inhaled albuterol (a bronchodilator), a placebo inhaler designed to mimic albuterol, or ‘sham acupuncture’—only albuterol...
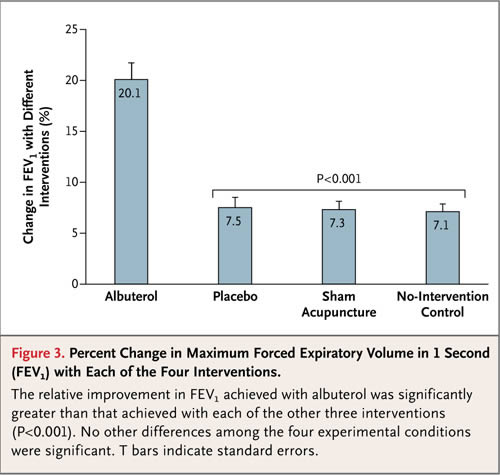
Spin City: Using placebos to evaluate objective and subjective responses in asthma
As I type this, I’m on an airplane flying home from The Amazing Meeting 9 in Las Vegas. Sadly, I couldn’t stay for Sunday; my day job calls as I’ll be hosting a visiting professor. However, I can say—and with considerable justification, I believe—that out little portion of TAM mirrored the bigger picture in that it was a big success. Attendance at...

