Tag: breast cancer

Estrogen Matters
Hormone replacement therapy in menopause is safer and more effective than we have been led to believe. A new book examines the evidence and sets the record straight.

Angelina Jolie’s surgeon peddles misinformation about…breast cancer!
Dr. Kristi Funk is a surgeon to the stars in Beverly Hills who operated on Sheryl Crow and Angelina Jolie for breast cancer. This year, she published a book about breast health and breast cancer. Unfortunately, it's full of misinformation and radical advice with little or no basis in science.
Alternative medicine kills cancer patients, “complementary” edition
By definition, alternative medicine has not been shown to be effective or has been shown to be ineffective. Thus, alternative medicine is ineffective against cancer and can best be represented as either no treatment at all or potentially harmful treatment. It is thus not surprising that cancer patients who choose alternative medicine have a higher risk of dying from their cancer. A...

ASCO endorses the integration of quackery into breast cancer care
In 2014, the Society for Integrative Oncology first published clinical guidelines for the care of breast cancer patients. Not surprisingly, SIO advocated "integrating" dubious therapies with oncology. Last week, the most influential oncology society, the American Society of Clinical Oncology (ASCO), endorsed a 2017 update to the SIO guidelines, thus endorsing the "integration" of quackery with oncology and paving the way for...

Why do some women refuse treatments for their breast cancer?
Adjuvant therapy after surgery, such as chemotherapy, hormonal therapy, and radiation therapy, has contributed to a 39% decrease in breast cancer mortality since 1989. Unfortunately, a significant number of women decline evidence-based adjuvant therapy. A recent study suggests that distrust of the medical system plays a significant role in such refusal.

Naturopathy vs. patients: Patients lose
Over the weekend, there was a news story describing two cancer patients treated by naturopaths in New Zealand. Both died, one almost certainly unnecessarily, the other after enduring more suffering than she likely had to. These tragic cases and others reminded me of why it is so appalling that so many physicians are "integrating" naturopathy into "integrative medicine." In reality, they are...

Alternative medicine kills cancer patients
By definition, alternative medicine has not been shown to be effective or has been shown to be ineffective. Thus, alternative medicine is ineffective against cancer and can best be represented as either no treatment at all or potentially harmful treatment. It is thus not surprising that cancer patients who choose alternative medicine have a higher risk of dying from their cancer. A...
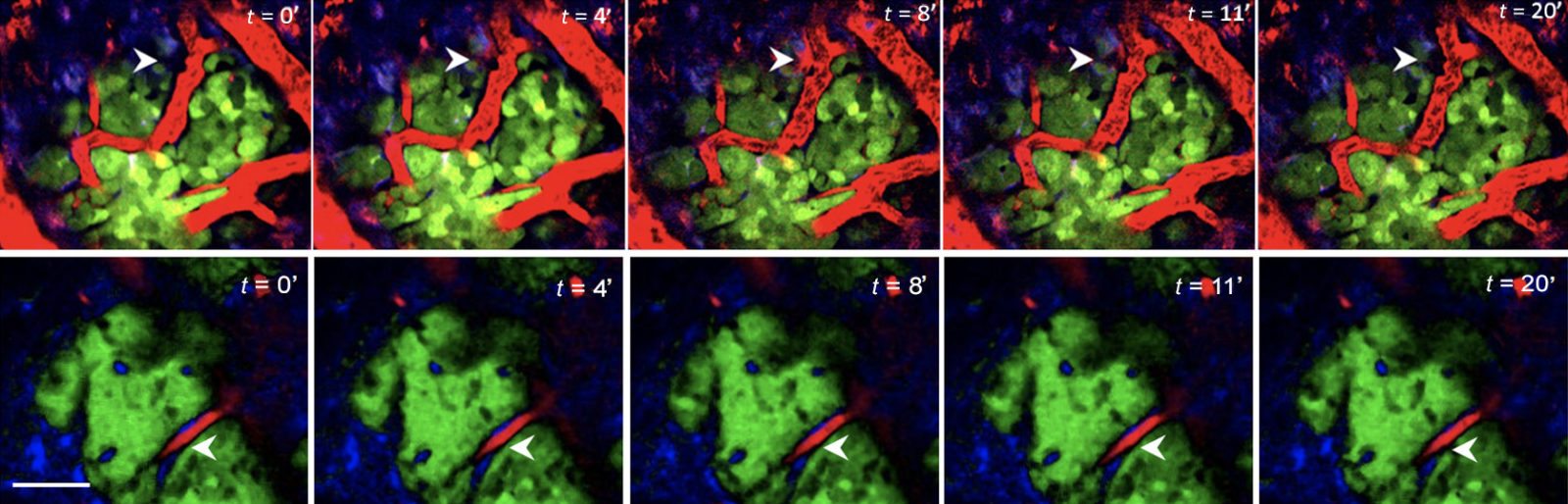
Does chemotherapy cause cancer to spread?
Earlier this month, a study was published in Science Translational Medicine that showed how chemotherapy before surgery can stimulate breast cancer invasiveness and invasion under certain circumstances. Not surprisingly, alternative cancer cure mavens everywhere are spinning the study as "proof" that chemotherapy has no benefit and causes only harm (and so you should buy their nostrums instead). Unsurprisingly, the actual results are...

Precision Medicine and Uncertainty
Precision medicine is a development that promises to tailor treatments to the individual patient based on genetic and other molecular and cellular analyses. In his 2015 State of the Union address, President Obama announced the Precision Medicine Initiative. A website for Precision Medicine claims to offer “perfect care for every individual.” Much of what we read about precision medicine gives the impression...
Mammography and overdiagnosis, revisited
Another new study supports the hypothesis that overdiagnosis is a major problem in mammography screening programs. Predictably, it is attacked based on a misunderstanding of what overdiagnosis is.