Tag: candida hypersensitivity
Of Mice and Men…and Coconut Oil
Editor’s note: This post is a collaborative effort between Grant Ritchey, a Science-Based Medicine semi-regular, and Stephanie Tornberg-Belanger, a co-author of the research paper discussed below and who brought the study to Grant’s attention. We are pleased to welcome Stephanie as a guest contributor to SBM. In his last SBM post, Grant reported on a systematic review of the literature that undermined...

Medicine doesn’t come from the hardware store: Don’t drink turpentine
I enjoy feedback from readers. Yes, there’s the regular hate mail accusing me of being a Big Pharma Shill. But there’s the occasional appreciative comment from someone that found a post helpful or informative. The most gratifying feedback is when someone tells me that something I wrote led to a more informed health decision. Often it’s because I was able to answer...
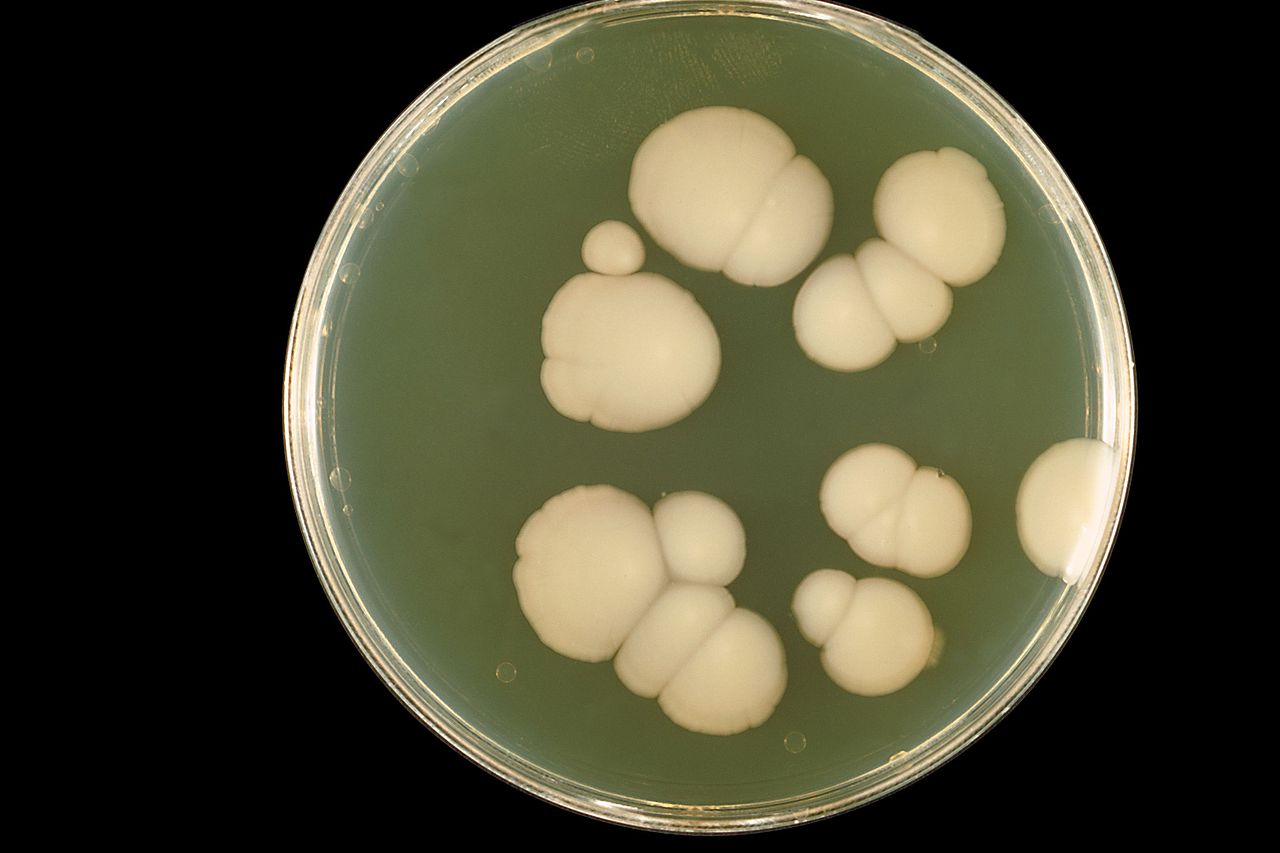
Candida and Fake Illnesses
While Big Pharma has been accused of inventing diseases, alternative medicine is the real champion of this practice. Compromised immunity can lead to overgrowth of the fungus Candida albicans, but this doesn't happen in people with intact immune systems, and it doesn't lead to the vague, unrelated symptoms described as "systematic candidiasis" by alternative medicine proponents.

