Tag: chiropractic stroke
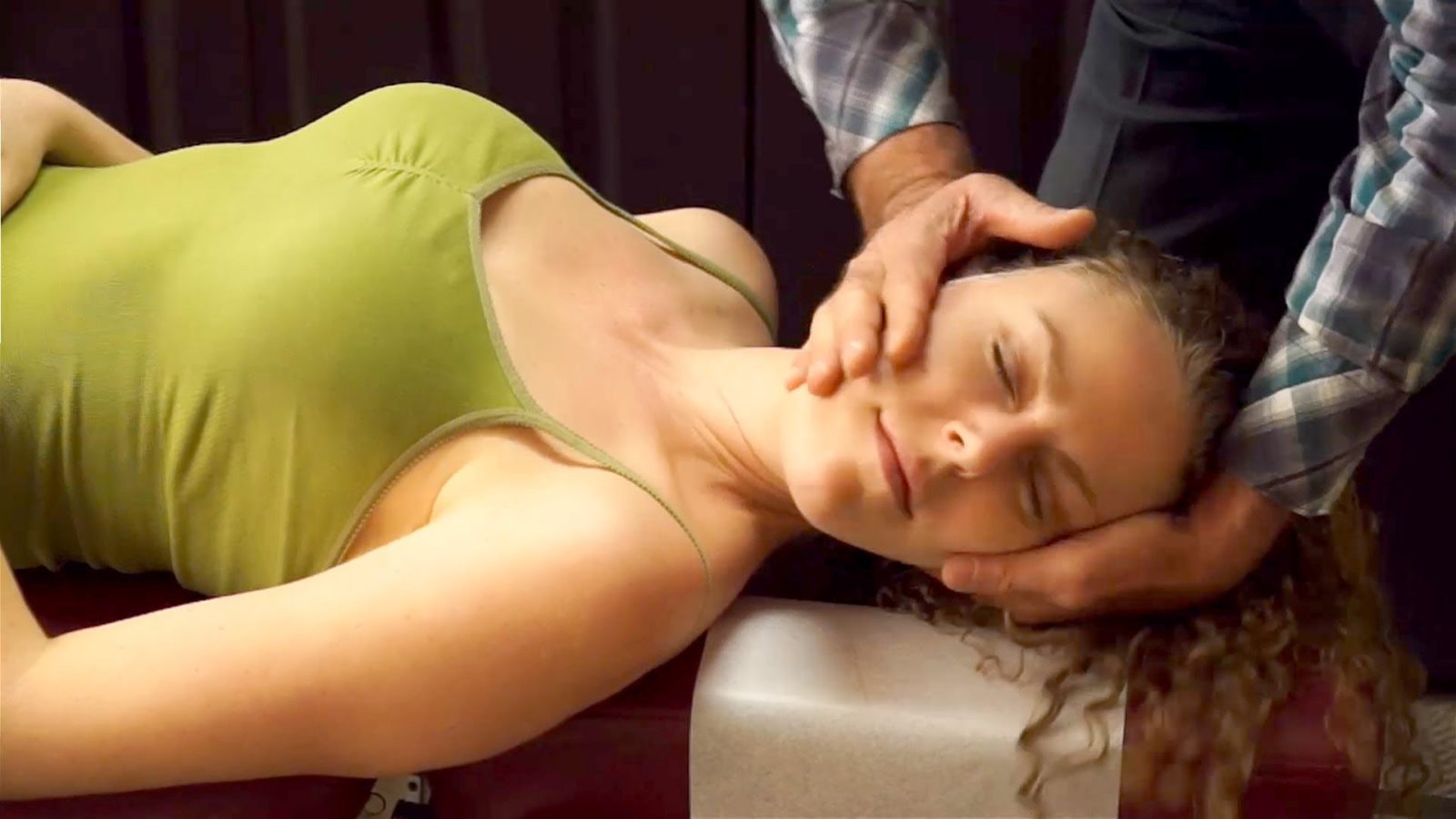
Study: patients should be warned of stroke risk before chiropractic neck manipulation
Another study adds to growing body of evidence that chiropractic neck manipulation is a risk factor for stroke. Patients should be warned of risk.
Cervicogenic Headache and Cervical Spine Manipulation
NOTE: Today we offer a double feature on the treatment of cervicogenic headache: this post and Dr. Harriet Hall’s post, “When Headaches Are a Pain in the Neck: Spinal Manipulation vs. Mobilization for Cervicogenic Headache.” They complement each other, as well as Dr. Hall’s post from last week on the possible risk of stroke with neck manipulation. A cervicogenic headache has been...
Chiropractic and Stroke: No Evidence for Causation But Still Reason for Concern
Can neck manipulation (by chiropractors or by other practitioners) cause strokes? Many of us think it can, but definitive proof is lacking. A recently published study looked at the available evidence. A systematic review found a small association between stroke and chiropractic care but concluded that the association was spurious and that there was no evidence for causation. My colleagues and I...
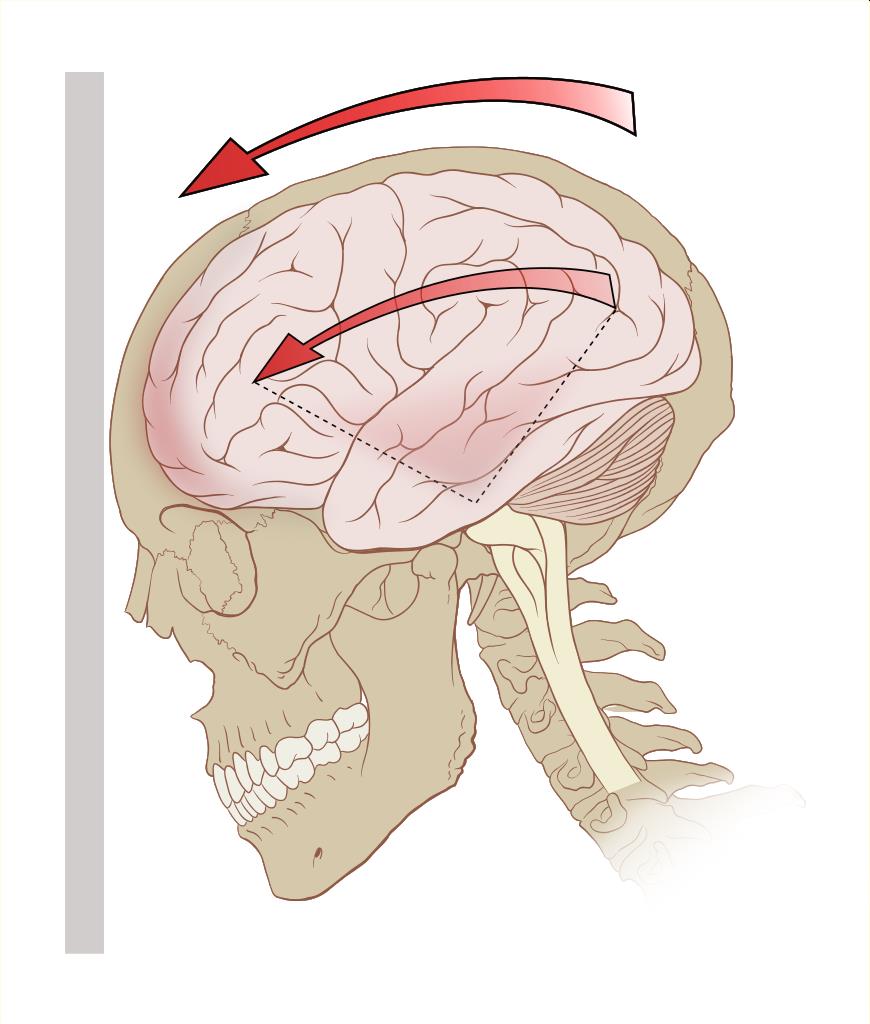
Chiropractors, Naturopaths, Concussions and Senate Bill 1535
Is it a good idea that chiropractors be allowed to clear children to play sports after a concussion? No. It is not a good idea.
Chiropractic and Stroke: The question is not answered
I am off to Chicago for 5 days to wow the SMACC crowd with my ID/SBM acumen. I hope. Given that most of my multiple-personalities do not seem to be able to get any work done, I am forced to write a brief post this week, limited by the battery life on my MacBook Air. Whatever I get down on paper? pixels?...
Chiropractic Manipulation of the Neck Linked to Stroke in a 6-Year-Old Child…
The risk of suffering a stroke when undergoing aggressive chiropractic manipulation of the neck is not a new concern. We’ve discussed it several times on the pages of Science-Based Medicine over the years, most recently in November of 2014 when Steven Novella covered the death by chiropractor of 30-year-old Jeremy Youngblood, whose fatal brain injury occurred while seeking treatment for a sore...

That’s so Chiropractic
Old bad studies: Fantastical autopsy results I found the following quote at “Chiropractic care can treat more than just bad backs” (FYI. Chiropractic can’t): Luse references a study published in The Medical Times authored by Dr. Henry Windsor [sic], M.D. that showcases the correlation of spinal health to overall wellness. Windsor dissected 75 human cadavers to investigate their causes of death. The...
Upper Neck Manipulation: Caveats for Patients and Providers
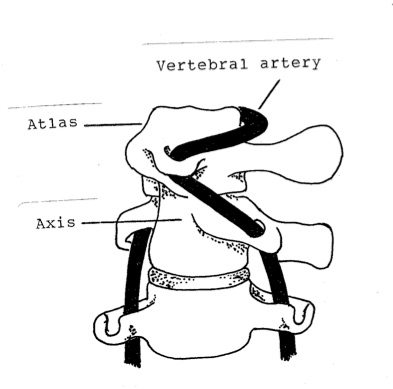
Chiropractors often deny that neck manipulation can be a primary cause of stroke by injuring vertebral arteries. But according to Jean-Yves Maigne, M.D., head of the Department of Physical Medicine at the Hôtel-Dieu Hospital in Paris, France: It is now a well established fact that cervical thrust manipulation can harm the vertebral artery. This accident was formerly regarded as very rare, although...