Tag: chiropractic

A Very Serious Book Review: The Heroic Adventures of Kid Ki’ro
An Australian chiropractor has written a children's book extoling the virtues of the profession in a most elliptical fashion.
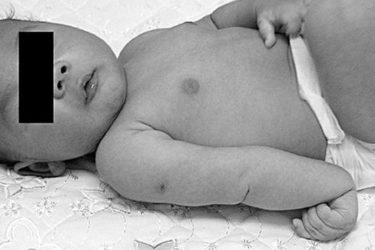
Chiropractic Care of an Infant with Erb’s Palsy: Another Worthless Case Report
A recently published case report claims that chiropractic care helped heal an infant's paralyzed arm. In reality, the chiropractor took credit for the natural course of a well-known medical condition and luckily didn't make things worse for the patient.

A New Study Finds No Benefit from Chiropractic for Infant Colic, but They’ll Keep Doing it Anyway
A new study attempted to answer the question of chiropractic's potential benefit for infant colic. It was successful, but I don't think it turned out the way the authors' hoped. Sadly, I don't think that this will change the mind of any chiropractor who treats babies.

Science-Based Satire: More Chiropractors are Using Subluxation Sniffing Dogs
Are dogs being trained to detect subtle chiropractic subluxations? If so, can they really outperform the Subluxatron 9000-X? And what about cats? These questions and more won't be answered by this post, because it's clearly satire and doesn't represent reality or even the opinions of the managing editors of this website.
The risks associated with alternative medicine
In a new paper, the types and severity of harms from different types of alternative medicine are described.

H.R. 2654 forces Medicare to treat chiropractors and MDs as equals
Chiropractors are deceptively trying to sell H.R. 2654 as expanded Medicare coverage for musculoskeletal conditions. The bill actually mandates that Medicare treat chiropractors and medical doctors as equals, covering anything a chiropractors are authorized to do under their expansive state scope of practice laws.
Science-Based Satire: Implantable Desubluxators Revolutionize Chiropractic Care
Have chiropractic scientists developed an implantable device that will detect and treat subluxations? Are there companies that monitor these devices in order to alert patients and to arrange for 24-7 emergency adjustments? No. There absolutely are not. This is satire.

The Guardian and the “Cult” of Online Chiropractic
Over the past few years, a handful of chiropractors have gone viral because of aggressive neck adjustments that make a loud crack and provide a quick thrill for viewers of their YouTube videos. A recent article in The Guardian discussed the phenomenon, but it doesn't go far enough.

Chiropractic, Chiropractic for Kids, and a Few of My Greatest Hits
A few thoughts on chiropractic and the evolution of my feelings on the subject. Also, a bit of a walk down memory lane with highlights of my most memorable posts on pediatric chiropractic quackery.


