Tag: cirrhosis
Separating Fact from Fiction in the Newborn Nursery: Hepatitis B Vaccine for Newborns
For those of you new to Science-Based Medicine, I am a pediatric hospitalist and spend the majority of my time caring for newborns. It’s an extremely rewarding experience on most days. The babies are usually healthy, the parents are usually happy and appreciative, and I get to give a lot of good news. I also get to dispel a lot of myths...
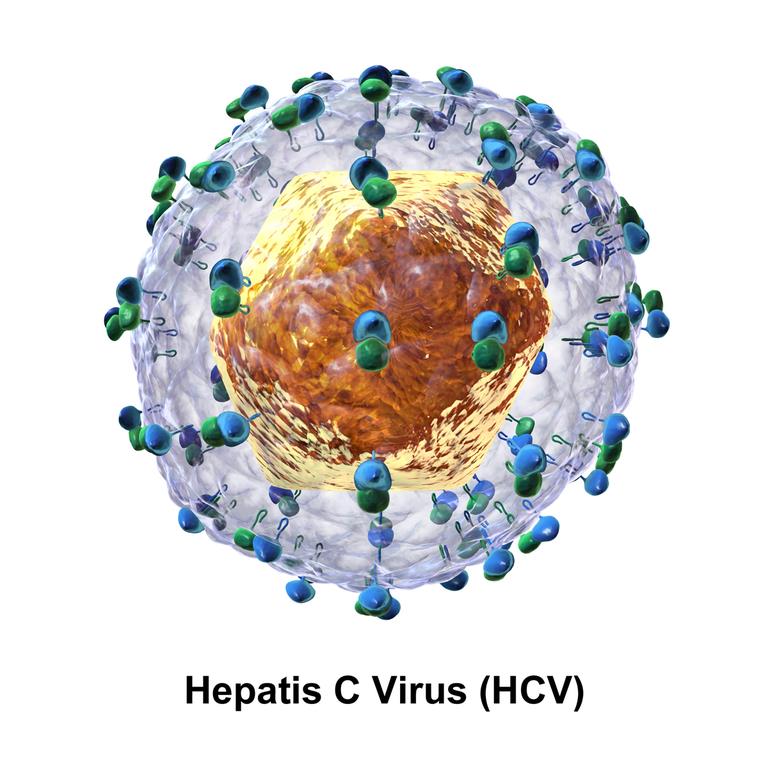
Curing Hepatitis C: A Success Story and a Price Tag
Previously incurable, hepatitis C now has a treatment. A very, very expensive treatment. But there is hope for acutely and chronically infected people.

