Tag: homeopathy

Confronting homeopathy, naturopathy, homeopathy, and other quackademic medicine at my alma mater
Several years back, I was forced to confront quackery at my alma mater in the form of an anthroposophic medicine program at the University of Michigan. The situation has deteriorated since then, as now the Department of Family Medicine there is inviting homeopaths to give talks and teaching acupuncture as credulously as any acupuncturist. Will the disease metastasize to other departments in...

Angelina Jolie’s surgeon peddles misinformation about…breast cancer!
Dr. Kristi Funk is a surgeon to the stars in Beverly Hills who operated on Sheryl Crow and Angelina Jolie for breast cancer. This year, she published a book about breast health and breast cancer. Unfortunately, it's full of misinformation and radical advice with little or no basis in science.
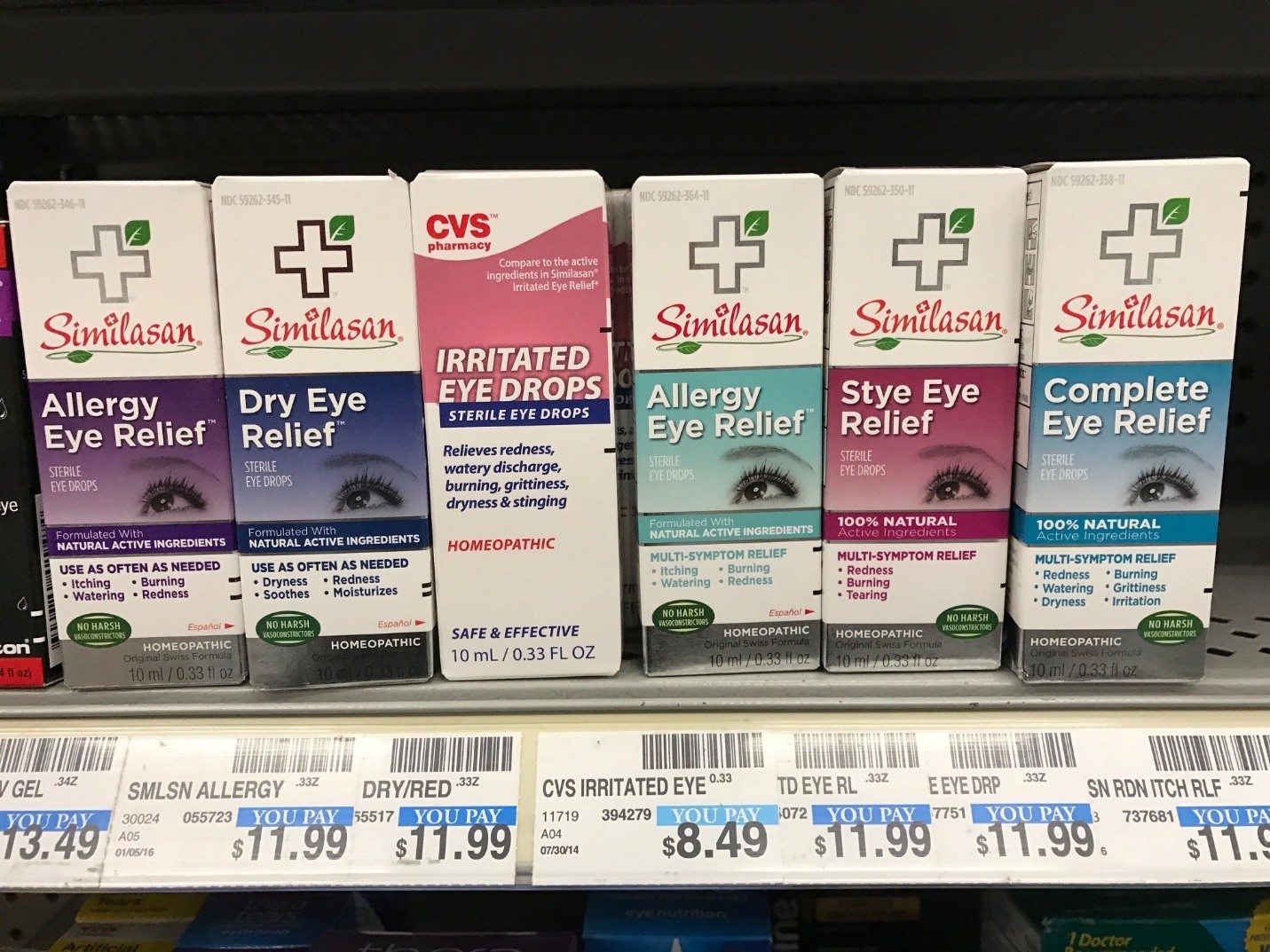
CVS sued for deceiving consumers in sale of homeopathic remedies
A lawsuit claiming pharmacy giant CVS fraudulently deceives consumers in the sale of worthless homeopathic remedies has been filed by the Center for Inquiry (CFI), acting on behalf of the general public. CFI says co-mingling ineffective homeopathic products with science-based treatments on CVS's retail shelves and online confuses consumers.
Homeopathic Arnica in Plastic Surgery
Homeopathic Arnica is clearly pseudoscience and does not work for wound healing, so why are so many cosmetic surgeons recommending it?

CEASE therapy for autism: Homeopathic quackery and “self regulation” by naturopathic boards
Naturopathy is quackery. If you doubt this, consider that you can't have naturopathy without homeopathy. What's even worse is when naturopaths subject autistic children to quackery like CEASE therapy. Expecting any naturopathic regulatory board to investigate quackery in naturopathy is the proverbial fox guarding the henhouse.

The Null hypothesis: Gary Null attacks science-based medicine
Over the last couple of weeks, one of the old men of quackery, Gary Null, has decided (yet again) that he really, really doesn't like science-based medicine. That includes Steve Novella, Susan Gerbic, and...me. As is his usual habit, Null teamed up with his producer Richard Gale and wrote some seriously off-base screeds against Wikipedia, skeptics, and science-based medicine, basically the forces...

Homeopathy, rabid dogs, and naturopathic propaganda
Last week, a story of a bizarre homeopathic remedy used by a Canadian naturopath made the news. Today, American naturopaths are in Washington, DC lobbying for increased prescribing power, including for controlled substances. Lawmakers should be reminded of the quackery at the heart of naturopathy.

How rabid dog saliva became an approved and endorsed remedy in Canada
A recent blog post by a British Columbia naturopath is raising questions from health professionals about the practice of naturopathy, and the use of homeopathic remedies to treat children with serious behaviour problems.

Homeopathy Awareness Week shows that homeopathy is still a problem
Homeopathy Awareness Week might be almost over, but The One Quackery To Rule Them All wastes resources and endangers patients year round, and a recent French criticism of homeopathy has provoked another case of legal thuggery by homeopaths.

The deadly false hope of German alternative cancer clinics
We at SBM have written about German cancer clinics that offer a combination of cancer quackery, some real medicine, plus unproven experimental therapies, all at a high cost, both financially and in false hope. Finally, an exposé of these clinics has been published. What these clinics are doing is even worse than even we had feared.

