Tag: pseudoscience
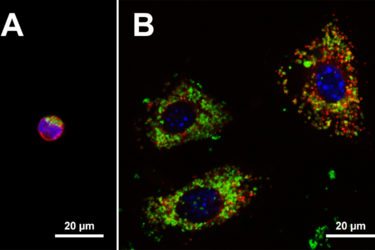
Move over, Christopher Shaw, there’s a new antivaccine scientist in town
Move over, Christopher Shaw, there's a new antivaccine scientist dedicated to demonizing aluminum adjuvants in town. His name is Christopher Exley. He's got a fluorescence microscope, and he's not afraid to use it.

ASEA – Still Selling Snake Oil
ASEAs marketing practices, in my opinion, are clearly deceptive. They use a lot of pseudoscientific claims representing the epitome of supplement industry misdirection and obfuscation. They use science as a marketing tool, not as a method for legitimately advancing our knowledge or answering questions about the efficacy of specific interventions.

Chiropractic and Spinal Manipulation Red Flags: A Comprehensive Review
Many people visit chiropractors’ offices seeking relief from back pain. Appropriate use of spinal manipulation provided by a chiropractor can be helpful in treating mechanical-type back pain, but there are good reasons to avoid chiropractic manipulation based on correction of “vertebral subluxations,” and there are red flags to look for before undergoing any kind of manipulative treatment for neck or back pain.

Acupuncturist Complains About Wikipedia
An acupuncturist complains about Wikipedia, saying it is under the control of self-styled skeptics who bias the content and bully anyone who disagrees. She only demonstrates her own bias; Wikipedia had good reason to ban her from editing.
Two (now retracted) studies purporting to show that vaccinated children are sicker than unvaccinated children show nothing of the sort
Antivaccine websites have been touting two recently published studies as strong evidence that vaccinated children are less healthy than unvaccinated children. The studies are so flawed that they show nothing of the sort. Even more hilariously, the bottom-feeding predatory open access journal that published them appears to have retracted them.

Russian Academy of Sciences Calls Homeopathy Pseudoscience
That homeopathy is pure pseudoscience is not news. Its basic principles are essentially magic, and the preparation of homeopathic products is indistinguishable from brewing a magic potion. Its two core principles, as the commission states, are a priori dogma - that like cures like, and that diluting substances out of existence leaves behind their magical essence. Science has progressed over two centuries...

Corrigendum. The week in SBM for 1.22.2017
Not every article and study that pops up my feeds in the world of pseudo-medicine is worthy of a complete blog post. But they need to be noticed and commented upon: Liver toxicity from herbs. Popped lungs from acupuncture. Chiropractic does not help scoliosis. Yoga is just exercise. There are eight kinds of wind: Great Feathery Wind, Scheming Wind, Hard Wind, Great...

Medical science policy in the U.S. under Donald Trump
The election of Donald Trump was unexpected. Given Trump's history of antivaccine beliefs and conspiracy theories, coupled with a fervor for deregulation (a fervor shared by the Republican Congress), it is reasonable to fear what will happen to medical science policy during the next four years.

“Donald Trump’s presidential election win stuns scientists”
Scientists in the U.S. and from around the world are weighing in on Donald Trump’s election as the next president of the most powerful country on earth: Trump will be the first anti-science president we have ever had . . . The consequences are going to be very, very severe. Michael Lubell, director of public affairs for the American Physical Society in...


Infiltrative Pseudoscience
If you don't think that CAM is the enemy of science in medicine, then you don't understand CAM and its proponents. Don't be fooled by their marketing. They want a return to the pre-scientific days when health gurus could sell any snake oil they want at exorbitant prices, with any hyped claims that they want, without going through all that tedious science.