Tag: residency training
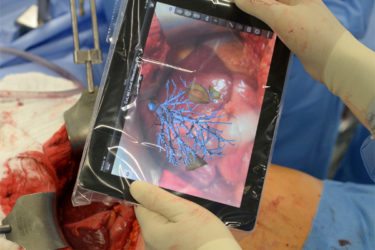
Augmented Reality in Medicine
Augmented reality has the potential to revolutionize how physicians access data while caring for patients, whether in the operating room or clinic.

Medical Profession is Underutilizing Computer Technology
There is tremendous potential to improve the medical industry through robust adoption of electronic systems for training and improving practice. So why aren't we doing it?
The elusive “potential” of integrative medicine
UPDATE: Dr. Katz has responded to this post in his usual venue, The Huffington Post. Alternative medicine was all about “potential” from the get go: In 1991, the Senate Appropriations Committee responsible for funding the National Institutes of Health (NIH) declared itself “not satisfied that the conventional medical community as symbolized at the NIH has fully explored the potential that exists in...

Naturopathic Medical Magic in the NW
As regular readers know, I live in the great Pacific Northwest, specifically Portland, Oregon. I am at home in the organic/hippy/environmental mind-set. It is what I grew up with. It is a relaxed, informal place to live. It is not much of an exaggeration to say that formal attire is tucking your tee shirt into your jeans. At least the metro area,...
Twenty days in primary care practice, or “naturopathic residency”
The metastasis of alternative medicine throughout the health care system comes, in no small part, at the hands of the federal and state governments, mostly the latter and most particularly the state legislatures. Under their jurisdiction rests the decision of who can, and cannot, become a licensed health care practitioner, and what they can, and cannot, do. This is the gateway through...
What Doctors Feel
Doctors are often accused of being unfeeling technicians who treat their patients like cases of disease rather than people (think Dr. House). We were taught in medical school to remain detached, not get too close to patients, and not show our emotions. That attitude was epitomized in William Osler’s essay Aequanimitas. But doctors have feelings like anyone else, and no one is...
Resident’s Working Hours- Should We Let Sleeping Docs Lie?
The Accreditation Council for Graduate Medical Education (ACGME) has released proposed new standards to limit working hours for medical residents. Bus drivers are allowed to drive for 10 hours and then are required to have 8 hours off duty. Airline pilots can be scheduled for up to 16 hours on duty — being at work, ready to fly — and up to...


Naturopathic Edumacation: A FAQ
An evaluation of a Naturopathic Education FAQ.