Year: 2012
No Health Benefits from Organic Food
A recent review of 240 studies has concluded that: The published literature lacks strong evidence that organic foods are significantly more nutritious than conventional foods. Consumption of organic foods may reduce exposure to pesticide residues and antibiotic-resistant bacteria. Organic produce has become increasingly popular in recent years. There are several reasons that consumers might prefer organic produce, including the belief that organic...
New AAP Policy on Circumcision
Back in 2008, I tried to look objectively at the scientific evidence for and against circumcision. I got a lot of flak from commenters who focused on the ethical issues rather than the scientific evidence. I concluded that the evidence showed small benefits and small risks, and I didn’t advocate either for or against the procedure. At the time, the American Academy...
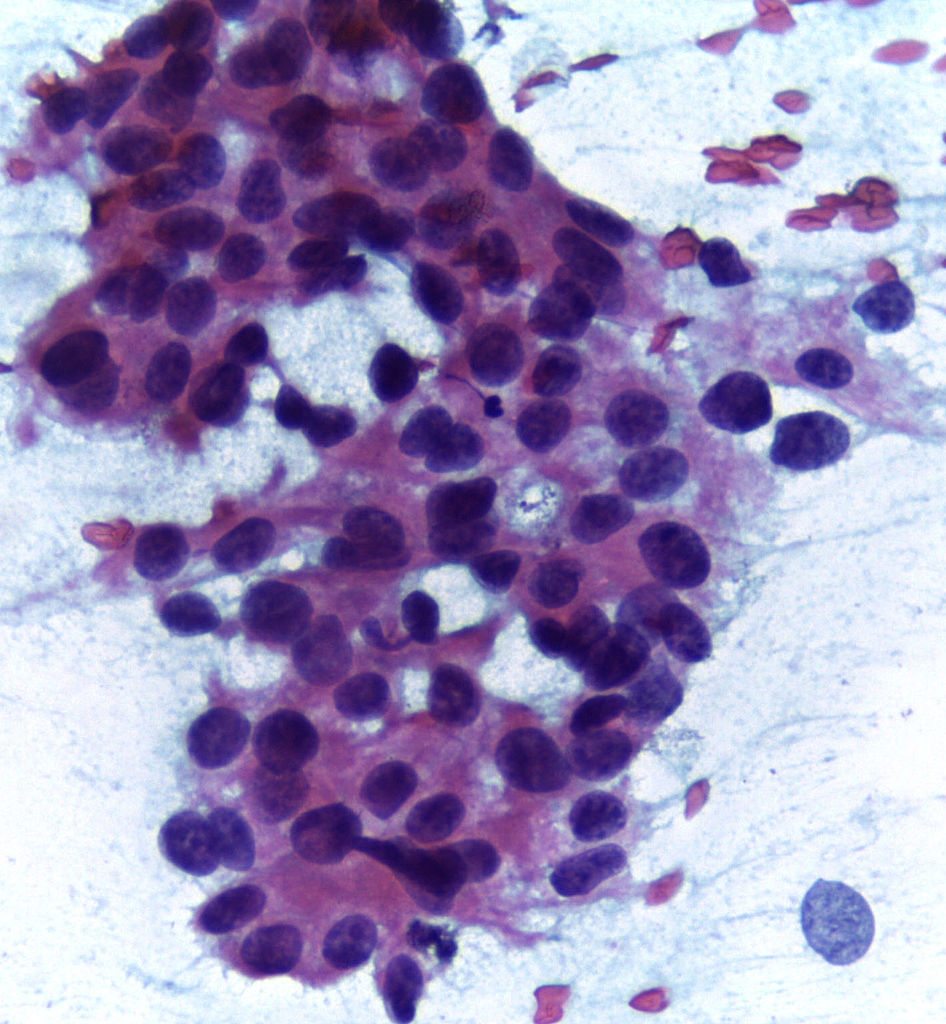
Alternative medicine use and breast cancer (2012 update)
[Editor’s note: It’s a holiday here in the U.S.; consequently, here is a “rerun” from my other super not-so-secret other blog. It’s not a complete rerun. I’ve tweaked it a bit. If you don’t read my other blog, it’s new to you. If you do, it’s partially new to you. See you all next week with brand spankin’ new material. It also...
Questioning Whether Psychotherapy and Support Groups Extend the Lives of Cancer Patients
What a wonderful world it would be if cancer patients could extend their survival time by mobilizing their immune systems by eating the right foods, practicing yoga, and venting their emotions in a support group. The idea that patients can enlist their immune systems to fight the progression of cancer is deeply entrenched in psychosomatic medicine and the imagination of the lay...

Rejecting cancer treatment: What are the consequences?
There have been several studies of people who have refused scientific treatments for cancer. The results have not been good.
The Power of Replication – Bems Psi Research
I love reading quotes by the likes of Karl Popper in the scientific literature. A recent replication of Bem’s infamous psi research, Feeling the Future, gives us this quote: Popper (1959/2002) defined a scientifically true effect as that “which can be regularly reproduced by anyone who carries out the appropriate experiment in the way prescribed.” The paper is the latest replication of Daryl Bem’s...
Andrew Weil’s Seasonal Supplements
Dr. Andrew Weil has teamed with Innate Response Formulas to develop a series of seminars and a line of products for “seasonally appropriate integrative strategies.” Seasonal Therapeutics is a system for adjusting diet supplement recommendations according to the season of the year. To kick off the program, a one-day seminar was presented by Weil’s colleague Tierona Low Dog in Boston on August...
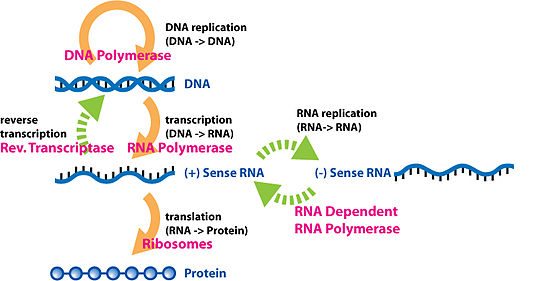
The “central dogma” of alternative/complementary/integrative medicine
There is something in molecular biology and genetics known as the “central dogma.” I must admit, I’ve always hated the use of the word “dogma” associated with science, but no less a luminary than Francis Crick first stated it in 1958, and it has been restated over the years in various ways. Perhaps my favorite version of the central dogma was succinctly...
Brief Announcement: Video of Panel on Alternative Medicine
Last month at JREF’s The Amaz!ng Meeting in Las Vegas, 3 SBM bloggers along with Rachael Dunlop of Australia participated in a panel on “The Truth About Alternative Medicine.” The video is now available on Youtube. It’s a chance for readers to see Steven Novella, David Gorski and Harriet Hall and hear them speak instead of just reading what they write.
Low Level Lasers: N-Rays in action.
I do not want to get all angsty and omphaloskeptic, but I have been thinking more of late about the purpose of the blog and my role in it. Blogs,and the people who write them, are ephemeral. It takes a unique personality and commitment to churn out these essays and commit them to the ether. Especially since Michelson and Morley. I have never...

