
The Baloney Protection Act
We have had to endure a great deal of interference from government in the conduct of institutions that should be governed by science and evidence. I’m sorry to report – here is one more. Senators Mike Lee (R-UT) and Tommy Tuberville (R- AL) have recently introduced a bill that would limit the FDA’s ability to regulate the blatant pseudoscience of homeopathy. This...

Sabotaging America’s Future: The Catastrophic Cost of Federal Research Cuts
The gleeful efficiency of an arsonist who mistakes the blaze for proof of his power

Will NIH Director Jay Bhattacharya stand up for scientists censored by the American Diabetes Association?
Last Friday, the American Diabetes Association censored diabetes researchers at its annual meeting who opposed the Trump administration's NIH policies. Will "Flame of Freedom" winner Jay Bhattcharya speak up?

Reason’s Next “Flame of Freedom” Winner Should be Someone Who Stood Up to Their Past “Flame of Freedom” Winner, Dr. Jay Bhattacharya
Reason staff and donors richly deserve to listen to a thorough, honest appraisal of everything their past "Flame of Freedom" winner is doing to free speech today. Perhaps it will dawn on some of them that they promoted fake censorship to bring about the real thing.

The Authors of the Book “The War on Science” Won Their War. Are They Happy Now?
Trans people are literally on the run and research into topics our government deems “DEI” is verboten. Has this ushered in a golden era of open scientific research and discovery?

The COVID Amnesia Project: Erasing Your Free Will to Preserve the Fantasy of the Optional Pandemic
Countless millions of Americans prioritized their health and protecting their neighbors over an imagined return to normal in 2020. Our sacrifices deserve recognition and gratitude, not amnesia and revisionist history from sheltered political scientists.
Revolutions in Drug Delivery
New medicines are getting better. But so is our ability to get them where they need to go.

In Animal Study, Nanobots Repair Spinal Cords
For my entire career as a neurologist the ability to repair an injured spinal cord has been one of the holy grails. There has always been promising new research that definitely increases our knowledge but doesn’t lead to an effective treatment. This is not for lack of trying – I also remember the period when Christopher Reeve was a tireless promoter of...
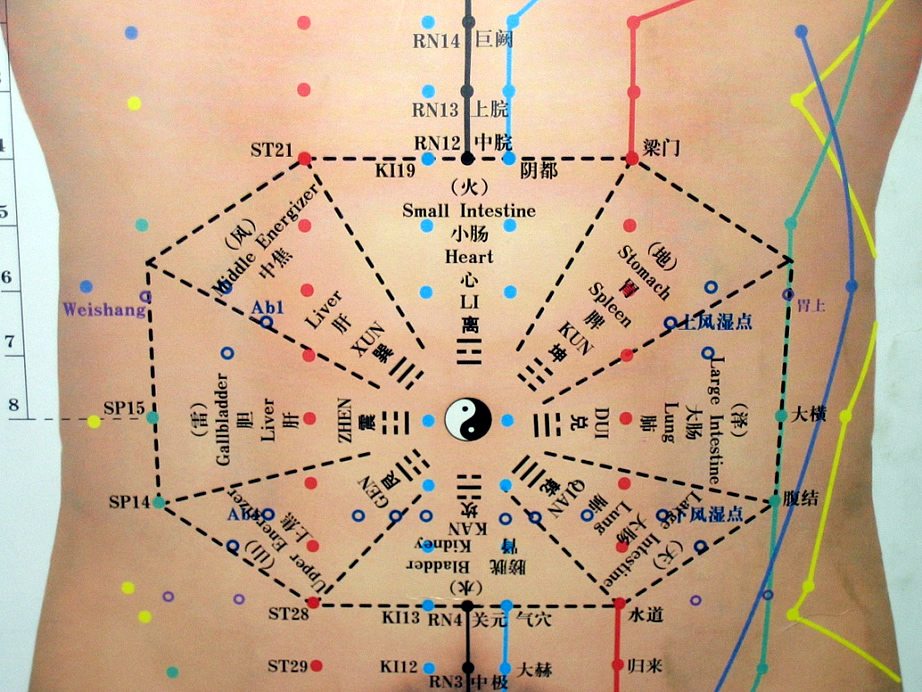
Acupuncture for Heart Attacks and more State-Sanctioned Pseudoscience
States default to a private organization run by acupuncturists and TCM practitioners to vet continuing education courses, with predictable results.

The Lysenko-ization of federal science takes a big step forward
From the beginning, Trump science policy has been Lysenko 2.0, in which ideology, not scientific promise and rigor, dictates federal grantmaking. OMB Director Russell Vought's proposed rules de-emphasizing peer review and placing political appointees in charge of final grantmaking decisions do Lysenko proud.




Sabotaging America’s Future: The Catastrophic Cost of Federal Research Cuts
The gleeful efficiency of an arsonist who mistakes the blaze for proof of his power