The Gene: An Intimate History
Six years ago I reviewed Siddhartha Mukherjee’s book The Emperor of All Maladies: A Biography of Cancer. It was hands-down one of the best books I have ever read on a medical topic. Now he’s done it again. His new book is titled The Gene: An Intimate History. Mukherjee is a superb writer. Much of what I said about his first book...
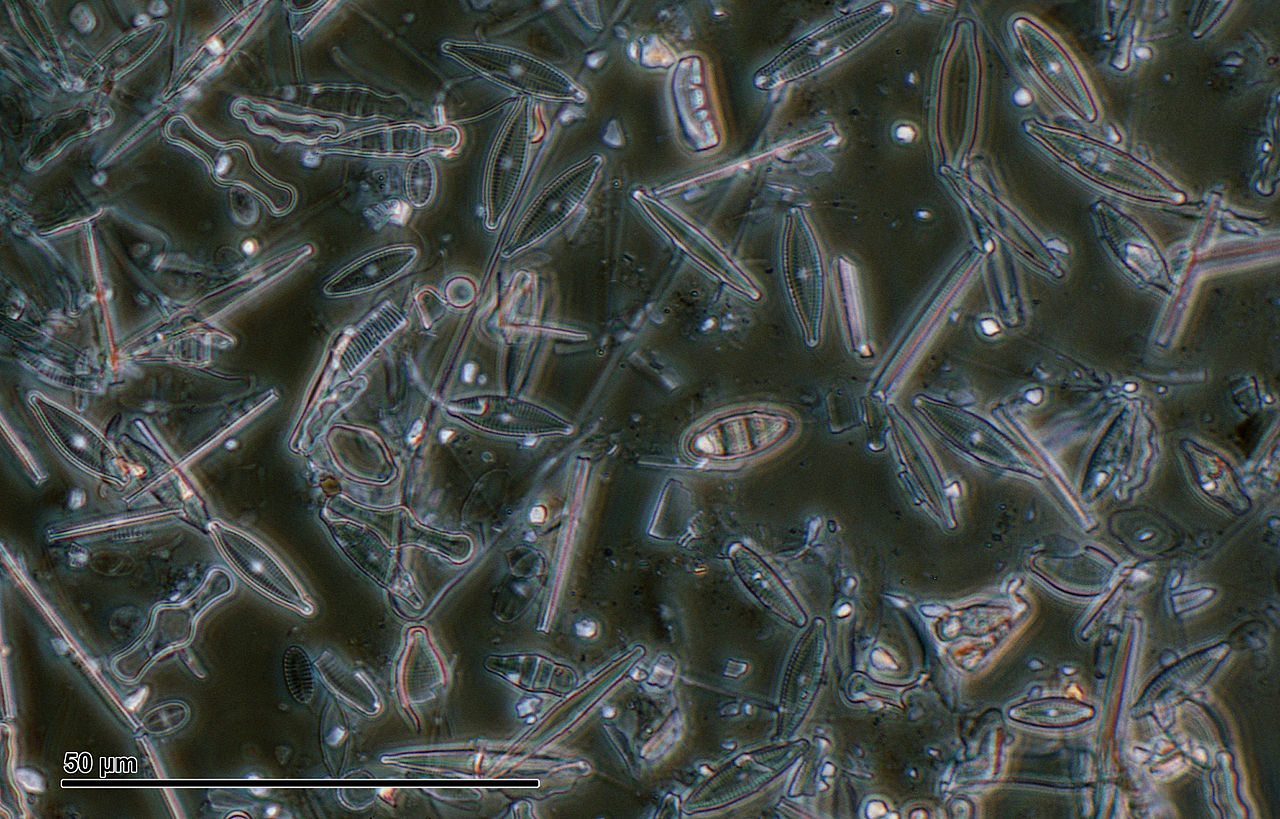
Diatomaceous Earth? No Thank You!
Diatoms are unicellular algae, one of the two major classes of the phytoplankton that constitute the bottom of the food chain in oceans and freshwater. Diatomaceous earth is a soft, siliceous sedimentary rock containing the fossilized skeletal remains of diatoms. It has been used as a bug killer: it is hypothesized that the sharp particles physically cut up the insects and also...

Vegan Betrayal: The Myths vs. the Realities of a Plants-Only Diet
NOTE: The original version of this book review was criticized for not making it clear when I was simply reporting the book’s content and when I was expressing support for one of its arguments. I have revised it to make it more clear. The additions are marked by brackets. Vegetarians come in several flavors. Ovo-vegetarians eat eggs, lacto-vegetarians eat dairy products but...

The THRIVE Experience: Masterful Marketing, Short on Substance
My daughter told me about the latest health fad among her group of acquaintances. She knows people who are spending $300 a month on the THRIVE program and claiming miraculous results. With a skeptic for a mother, my daughter knew enough to question the claims and do her own research; she was not impressed. She concluded that THRIVE was essentially selling caffeine...
Book Review Lagniappe
Lagniappe, a word often heard in New Orleans, refers to a bonus or extra gift, like the thirteenth donut in a baker’s dozen. You may have noticed that I write a lot of book reviews. I read far more books than I review, and I have always loved to read about the experiences of doctors and the interesting patients and intriguing illnesses...
The ROCA Screening Test for Ovarian Cancer: Not Ready for Prime Time
Ovarian cancer is relatively rare but deadly. The lifetime risk of ovarian cancer is 1.5% compared to 12% for breast cancer, but it is the 5th most common cause of cancer death for women. Since the ovaries are hidden deep in the pelvis and the symptoms of ovarian cancer are non-specific, the cancer is often advanced by the time it is diagnosed...
The Blood Cleaner: Invented by Ray Jardine
I recently heard about a man who was planning a hike in a tick-infested area and thought he could avoid Lyme disease by using Ray Jardine’s Blood Cleaner. Ray Jardine is a well-known mountaineer, rock climber, long-distance hiker, and outdoor adventurer. A lightweight hiking enthusiast, he has branched out into selling lightweight equipment like backpack kits, tarps, and insulated hats. Most of...
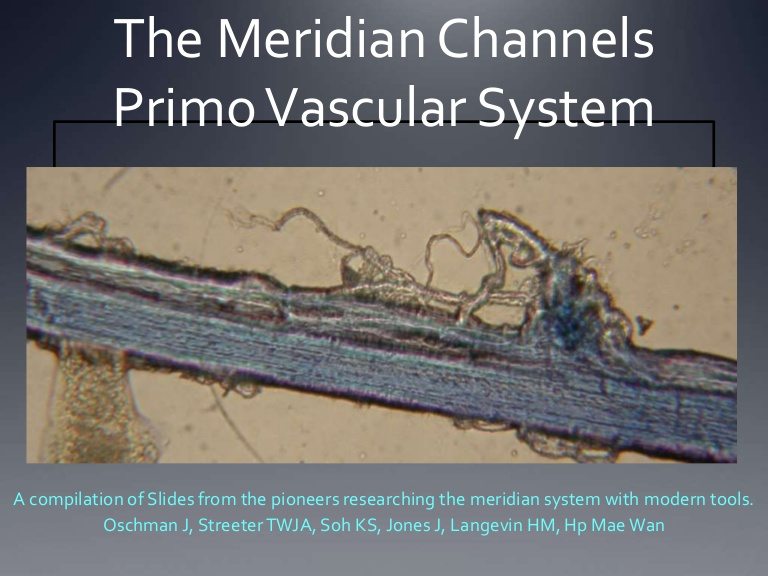
The Primo Vascular System: The N-rays of Acupuncture?
Acupuncture meridians and acupoints are imaginary until proven otherwise. Anatomists have never been able to detect them by microscopy or autopsy, and they are not mentioned in anatomy textbooks. For decades, acupuncturists have been trying to prove that their pre-scientific belief system is grounded in scientific reality. Now they are telling us that acupuncture meridians and acupoints have been discovered in the...
Therapeutic Touch Pseudoscience: The Tooth Fairy Strikes Again
A study out of Iran titled “Therapeutic touch for nausea in breast cancer patients receiving chemotherapy: Composing a treatment” was recently published in the journal Complementary Therapies in Clinical Practice. It is a great example of the Tooth Fairy science that permeates much of the research in complementary and alternative medicine. In Tooth Fairy science, researchers attempt to study a phenomenon without...
Uncertainty in Medicine
Medicine is an uncertain business. It is an applied science, applying the results of basic science knowledge and clinical studies to patients who are individuals with differing heredity, environment, and history. It is commonly assumed that modern science-based doctors know what they are doing, but quite often they don’t know for certain. Different doctors interpret the same evidence differently; there is uncertainty...

