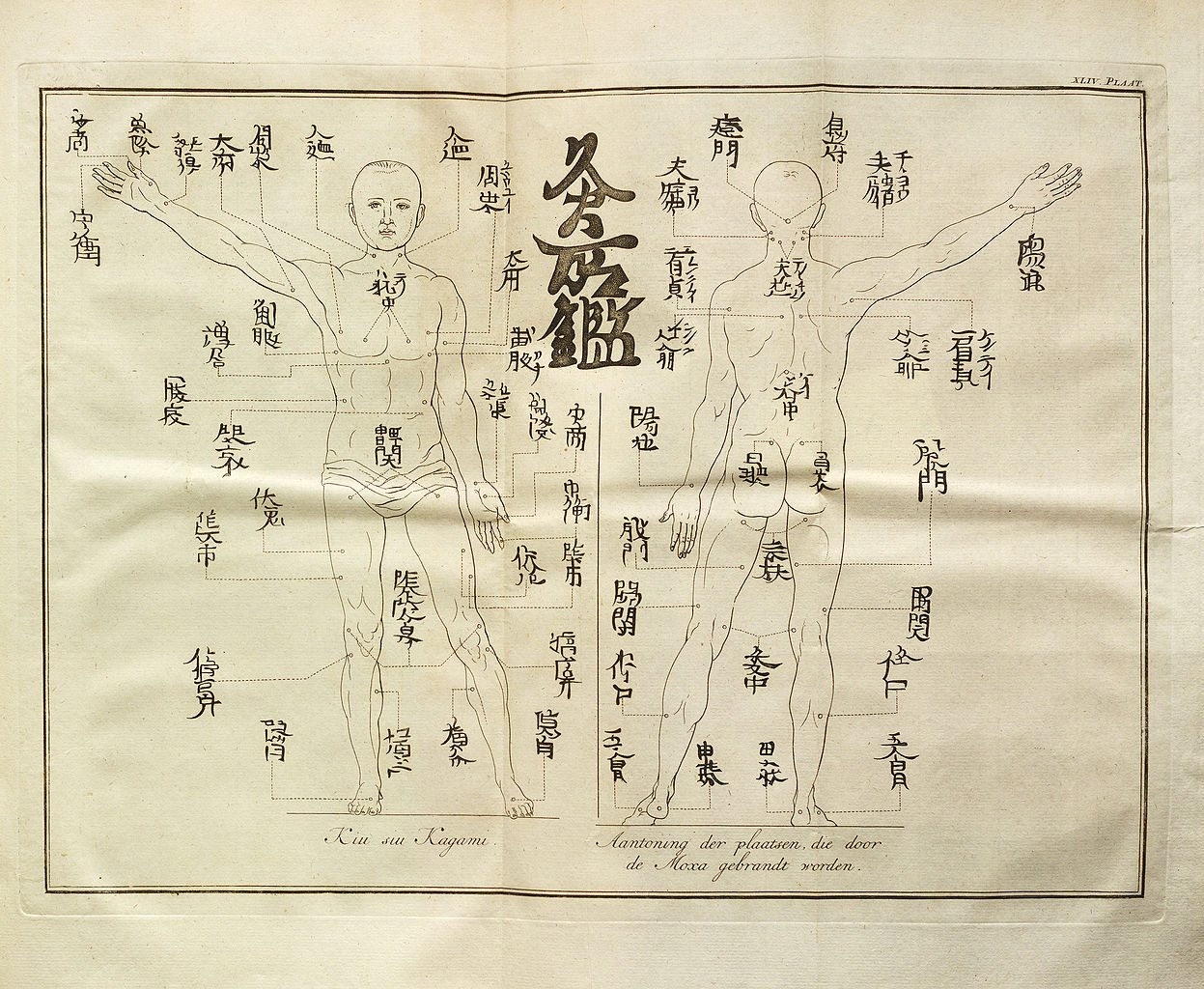
Systematic Review of Systematic Reviews of Acupuncture
No surprise - there is precious little evidence that acupuncture does anything.
Another Controversial Alzheimer’s Drug
A new treatment for Alzheimer's Disease is promising, but we're not there yet.
Don’t Forget About the Flu
We are heading into a bad flu season. Get vaccinated.
Study – For Lowering Cholesterol, Statins Work, Supplements Don’t
A study comparing a statin drug and six common supplements to placebo shows that only the drug lowers bad cholesterol.
Risk of Myocarditis Following COVID-19 Vaccine
Risk of myocarditis following mRNA vaccines is real but tiny, and far outweighed by the benefit of vaccines.
The Subvariants Are Coming
A wave of Omicron subvariants are coming. So get vaccinated.

Sleep Duration and Health
Poor sleep is a genuine concern, but the results of a new cohort study are complex to interpret.

Burden of Proof Studies and Health Risk
A new way of presenting knowledge about health risks highlights the ambiguity of the evidence and the importance of basic health behaviors.



The Effect and Future of Telehealth
The rapid adoption of telehealth caused by the pandemic has turned out to be a very positive thing.