Category: Neuroscience/Mental Health

Patients Who Deceive
Loren Pankratz's book Patients Who Deceive covers the whole spectrum of different kinds of deception. It is well written, informative, and entertaining, with case examples that read like detective stories.
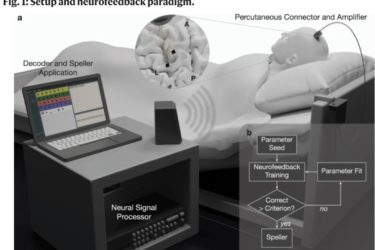
Paralyzed Patient Communicates with Brain Implant
Brain-machine interfaces continue to advance.

Facilitated Communication Is Still Pseudoscience
Facilitated communication is a harmful pseudoscientific technique that has managed to survive through rebranding and deception.

The World’s First Productivity Drink
Magic Mind claims to be the world's first productivity drink. There's no supporting evidence.
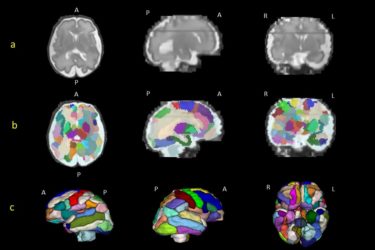
Fetal Signs of Autism
More evidence that ASD is a developmental disorder that begins in the womb.

Videos Said to be “Proof” that Nonverbal Autistics Can Communicate by Spelling
The father of nonverbal autistic child believes videos constitute proof that other children with autism can communicate by by pointing to letters on a board held by a facilitator to spell out words. He is wrong.

Antivaxxers misuse the Defense Medical Epidemiology Database to demonize COVID-19 vaccines
Over the last couple of weeks, a claim that the Defense Medical Epidemiology Database (DMED) shows that COVID-19 vaccines have caused a massive increase in cancer, neurological, and cardiovascular diseases in military personnel has gone viral. A closer look shows that the increases are almost certainly spurious and due to underreporting in previous years.

Using AI Technology To Treat Mental Illness
AI will likely play a big role in treating mental illness in the future, but quack uses are also likely to proliferate.

Culture-Bound Psychosomatic Syndromes
In her book Sleeping Beauties, neurologist Suzanne O'Sullivan travels the world to investigate fascinating stories of mass psychogenic illness where social and cultural factors result in symptoms that give voiceless people a way to be heard.
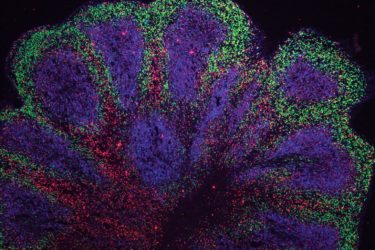
Mini-Brains for Disease Research
New research on organoid "mini-brains" highlights the potential of this new kind of scientific research.

