Category: Neuroscience/Mental Health
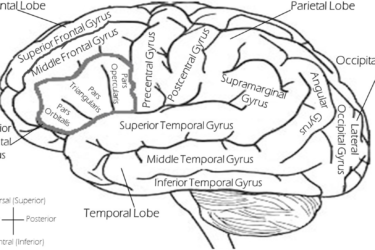
Neuriva: Clinically Proven?
Neuriva claims to have proof from clinical studies. That's misleading.
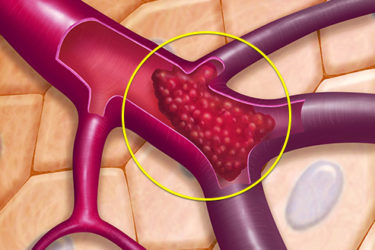
Stroke in COVID-19 Patients
A case series of five patients with COVID-19 and young strokes sparks many questions.

Tension and Trauma Releasing Exercises (TRE)
TRE exercises can supposedly cure PTSD by inducing tremors. Not credible. And there's no science to support the claims.

A miracle cancer prevention and treatment? Not necessarily as the analysis of 26 articles by legendary Hans Eysenck shows.
A recent investigation at King's College London has revealed major problems in the scientific career of one of psychology's most published scientists, Hans Eysenck.
AARP report: Insufficient evidence that dietary supplements benefit brain health
Experts convened by the AARP say don't waste your money on dietary supplements claiming they improve brain health. A healthy diet and lifestyle are the best medicine for your brain.

Decision Against Spelling to Communicate – A Small Victory for Science
Spelling to Communicate is just another form a facilitated communication, an invalid technique that was disproved decades ago but refuses to die.

Virtual Reality Treatment for PTSD
What does the evidence say about using virtual reality to treat PTSD?

Holotropic Breathwork
Holotropic breathwork is essentially voluntary hyperventilation, and old technique gaining in popularity as a way of generating "spiritual" experiences.

Improving mental health is a walk in the park (but mind the volcanoes)
Using Twitter and geotagging, researchers add to the growing body of evidence demonstrating an association between contact with nature and improved mood.


