Category: Surgical Procedures
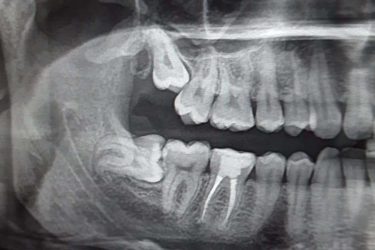
The Wisdom of Third Molar Removal
In the Olden Times (ten or so years ago), the indication for third molar (aka “wisdom teeth”) removal was the presence of wisdom teeth. Now, oral surgeons are rethinking things.
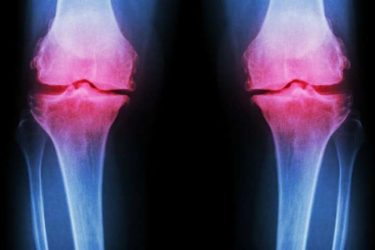
Stem Cells for Knee Arthritis
Stem cell treatments for knee arthritis are not yet ready for prime time, but that has not stopped their premature commercialization.
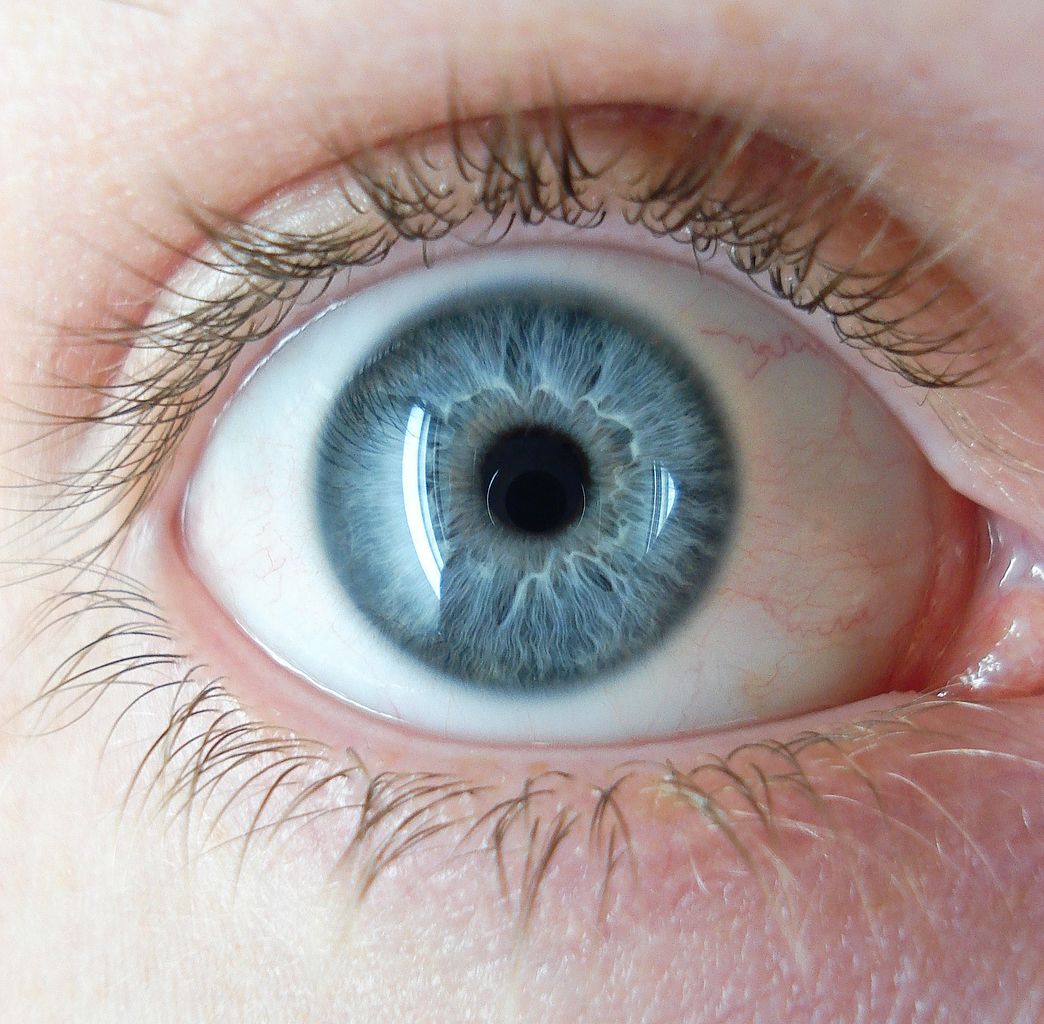
Patients blinded by stem cell therapy: an update
An update on the tragic results of unproven stem cell treatments to treat macular degeneration.
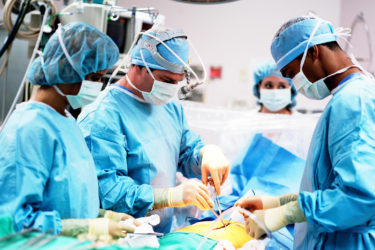
Bouffant caps versus skull caps in the operating room: A no holds barred cage match
Over the last few years, AORN and the American College of Surgeons have been battling it out over AORN's 2014 guideline that has increasingly led to the banning of the surgical skull cap in the operating room in favor of the bouffant cap. Lacking from this kerfuffle has been much in the way of evidence to support AORN's guideline, but unfortunately that...
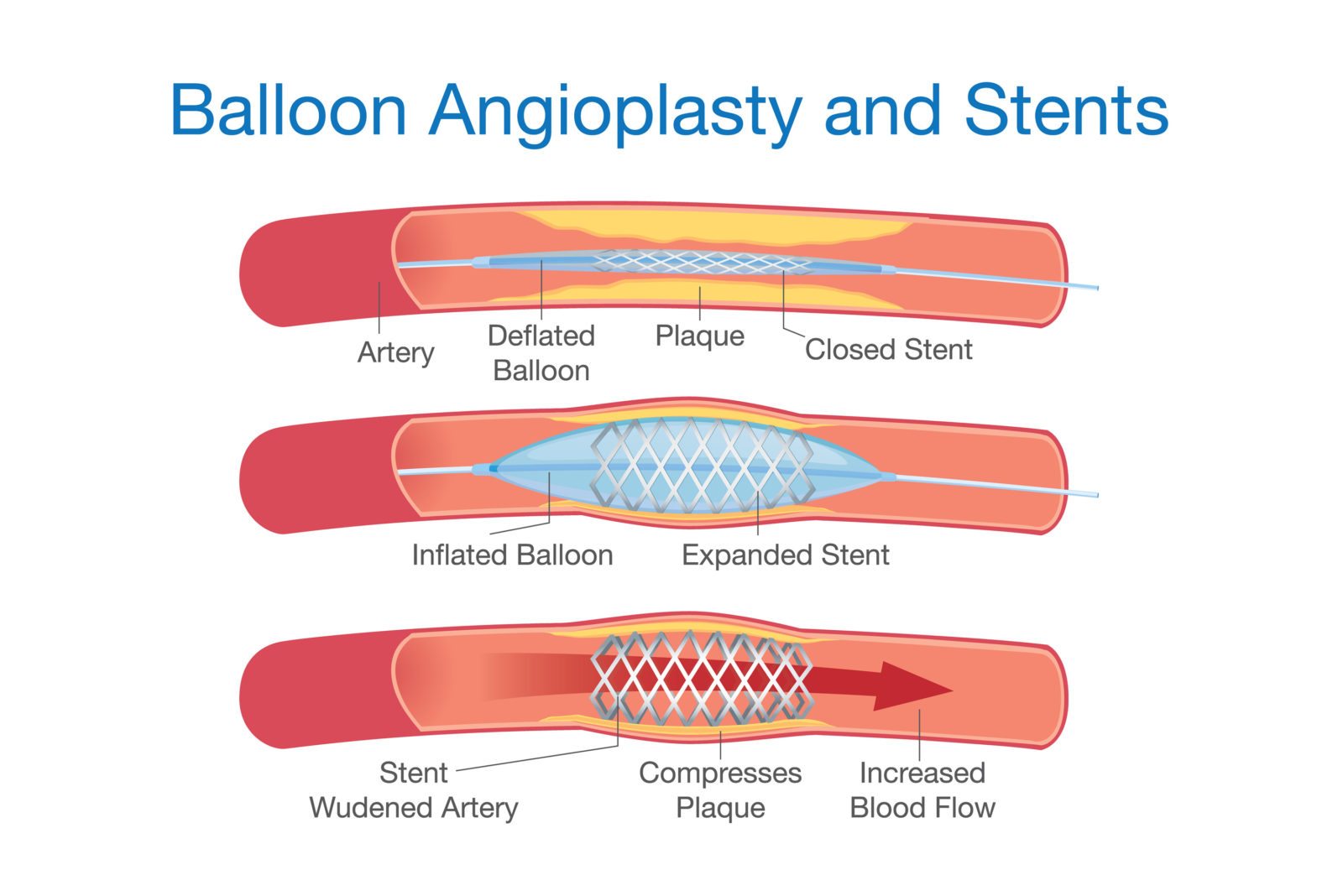
ORBITA: Another clinical trial demonstrating the need for sham controls in surgical trials
Last week, the results of ORBITA were published. This clinical trial tested coronary angioplasty and stenting versus optimal medical management in patients with single-vessel coronary artery disease. It was a resoundingly negative trial, meaning that adding stenting to drug management didn't result in detectable clinical improvement. What was distinctive about this trial is that it used a sham procedure (i.e., placebo) control,...

Naturopaths are fake doctors cosplaying real doctors (even the ones running dubious stem cell clinics)
Naturopaths are fake doctors who, increasingly, are cosplaying real doctors. Not surprisingly, because naturopaths go where quacking takes them, they've started to open their very own dubious stem cell clinics, thus combining the worst of both worlds, their "natural" quackery with dubious unproven but "high tech" treatments being peddled by the worst of real doctors.
In Pursuit of Patient Safety
[Editor’s note: With Dr. Gorski enjoying a vacation to recharge his batteries, we present a second offering from contributor James Thomas. Enjoy!] Advocates of CAM* (Complementary and Alternative Medicine) have long argued that mainstream medicine is a dangerous undertaking using toxic drugs and invasive interventions that often do more harm than good, while the various quackeries huddled under the CAM umbrella are...
Carotid Artery Stenosis: Surgery, Stent, or Nonsurgical Stroke Prevention?
The carotid artery in the neck is a common site of atherosclerosis. As plaque builds up, it leaves less room for blood flow and can cause strokes through clotting or embolization. Carotid stenosis is defined as a greater than 70% narrowing of the lumen (the space through which the blood flows in an artery). It can cause symptoms, including transient ischemic attacks...
The cost of repealing mandatory motorcycle helmet laws
It’s a seldom mentioned aspect of my professional history that I used to do a lot of trauma surgery in my youth. I did my residency at a program that included a county hospital with a busy trauma program where I saw quite a bit of vehicular carnage and an urban hospital (which has since closed) where I saw a fair amount...
You’ve been diagnosed with breast cancer. How soon do you need treatment?
Timely surgery for breast cancer is obviously better than delaying surgery, but how long can a patient safely wait for surgery once diagnosed. Because a randomized controlled clinical trial to answer this question would be unethical, this has been a difficult question to answer. Fortunately, a new study provides an estimate of how much of a delay it takes before outcomes start...

