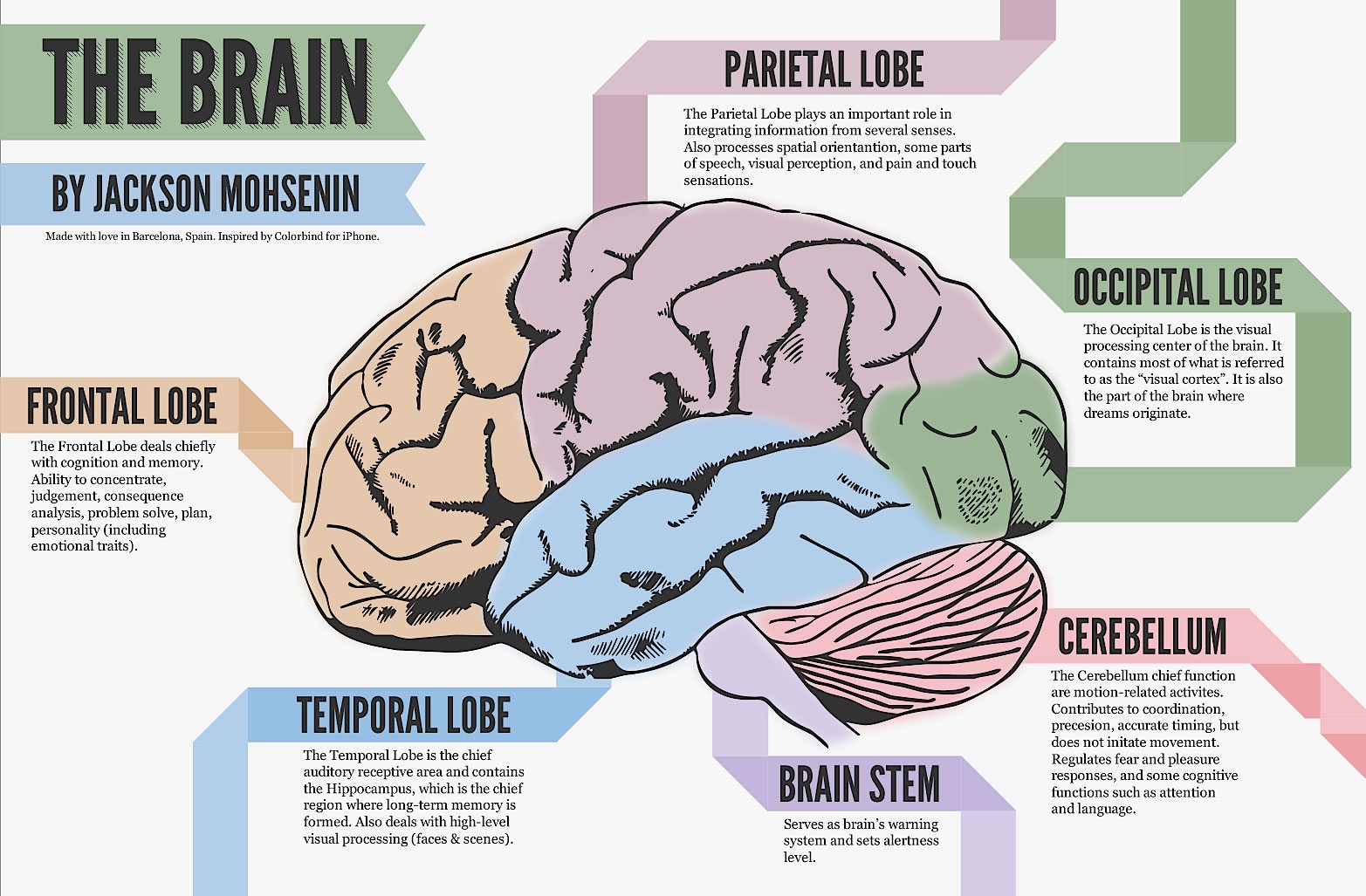
MEND Protocol For Alzheimer’s Disease
The medical profession is currently engaged in a simmering debate about what is the best overall approach to take toward the relationship between science and health care. I would say that the current dominant model is Evidence-Based Medicine (EBM). We, of course, advocate for a number of tweaks to EBM we call Science-Based Medicine (SBM). SBM essentially advocates for an ironic-sounding holistic...
The ROCA Screening Test for Ovarian Cancer: Not Ready for Prime Time
Ovarian cancer is relatively rare but deadly. The lifetime risk of ovarian cancer is 1.5% compared to 12% for breast cancer, but it is the 5th most common cause of cancer death for women. Since the ovaries are hidden deep in the pelvis and the symptoms of ovarian cancer are non-specific, the cancer is often advanced by the time it is diagnosed...

Whither the randomized controlled clinical trial?
With the rise of precision medicine and genomics, the conventional randomized clinical trial appears more and more outdated. Fortunately, clinical trials are evolving, but will it be enough to incorporate the numerous advances in "-omic" medicine in a rigorous scientific manner to benefit patients?
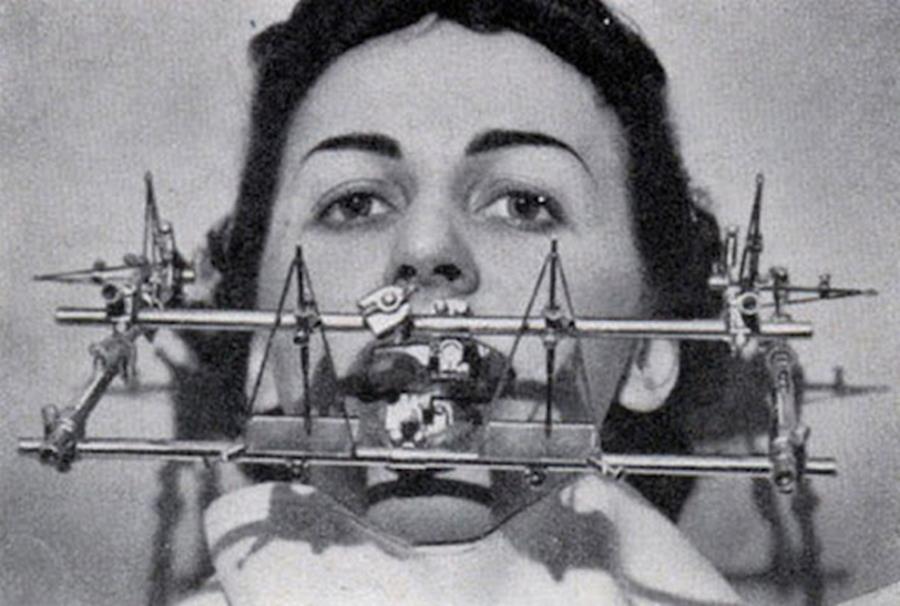
Use of Dental Appliances in the Management of Tourette Syndrome
Editor’s note: This Science Based Medicine blog post is another collaborative effort between Grant Ritchey and Clay Jones. Not only have they previously co-authored an SBM post on fluoride, their partnership has recently expanded into other areas of science journalism. Since the departure of Dr. Jason Luchtefeld as co-host of The Prism Podcast, Clay has joined Grant as the new co-host. To...

Bye Bye Bravewell
Exactly one year ago tomorrow, The Bravewell Collaborative shut down, an event so momentous that few seem to have noticed. It’s been a while since we at SBM devoted much attention to Bravewell, although, at one time, its doings were a regular feature of SBM posts. For those of you not familiar with Bravewell, a brief history. The main mover and shaker...
AMA Decides Gun Violence is a Public Health Issue
On June 14th the American Medical Association’s (AMA) House of Delegates in Chicago, IL voted almost unanimously to adopt a resolution supporting the idea that gun violence is a public health issue. The resolution also called for lobbying Congress to eliminate the ban on research into the causes of gun violence. The AMA reports: “With approximately 30,000 men, women and children dying...
The Blood Cleaner: Invented by Ray Jardine
I recently heard about a man who was planning a hike in a tick-infested area and thought he could avoid Lyme disease by using Ray Jardine’s Blood Cleaner. Ray Jardine is a well-known mountaineer, rock climber, long-distance hiker, and outdoor adventurer. A lightweight hiking enthusiast, he has branched out into selling lightweight equipment like backpack kits, tarps, and insulated hats. Most of...
Chiropractic Moves into Transportation
I debated which of two topics to blog about this week that appeared in my feeds. The first was “Graduate slams CQU for offering ‘pseudoscience degree’,” where an Australian is upset that her University is offering an undergraduate Bachelor of Science in Chiropractic and a postgraduate Master of Clinical Chiropractic degree because chiropractic is “complete pseudoscience”. And the second was: “Foundation for...






Don’t Blame the Patient