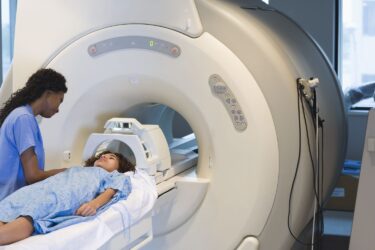
False balance in an NBC news story on whole body MRI scans
Over the weekend, NBC News aired a story on whole body MRI scans. Although it did include the usual cautions about false positives and the harm they cause, the caution was diluted by the story's focus a rare case of a woman who had a brain tumor detected. Overall, it was false balance that reminded me of vaccine/autism stories 20 years ago.

Science Based Satire: Sure, COVID Is Killing 1,500 Americans Per Week, But I Saw a Stranger Wearing a Mask…OUTSIDE!
We shouldn't "give a shit" about COVID. Instead, we should care deeply about strangers who still "give a shit" about COVID. They need to be publicly mocked and shamed over and over again.

Skeptics in the Pub: Cholera. Chapter 10a
When I woke up the next morning, I went for my usual tea and scone. Then I caught the trolley to work. When it reached the far side of the Steel Bridge, I hopped off. I took the steps down to the lower level and took the narrow walking path back across the river. I saw no one get off the trolley...
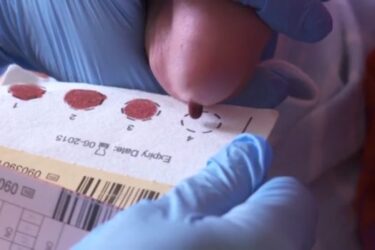
Music for Reducing Pain in Newborns
Newborns are exposed to painful procedures for good reason every day. Treating pain is important in this population, and music might play a role. At least it definitely won't hurt.

Adios Aduhelm
The controversial and never-proven-effective drug to treat Alzheimer's disease, aducanumab (Aduhelm) has been discontinued.

Mayo Clinic Promotes Reiki
The Mayo Clinic is a prestigious medical institution with a deserved international reputation. It also promotes rank pseudoscience. It does this, apparently, for all the reasons we have explored here at SBM over the years. I have seen first hand how one or a few true believers can promote so-called alternative medicine at their institutions, meeting little resistance from colleagues and administrators...

Yet more evidence that we physicians need to clean up our act
A recent study found that physicians and scientists who are perceived as "experts" are prevalent within the antivax community and more influential because of their status as physicians and scientists. Why do physicians continue to tolerate antivax quacks within our ranks?
Skeptics in the Pub. Cholera. Chapter 9b
“You are here early,” he said. “Yeah. I’m trying to decide what to do about this pump and the seawater cure. So far, my attempts are falling flat.” I told him about the couple pumping water and my lack of success in stopping them from taking the water home. “No surprise,” said Bonham. “Water is supposed to be as safe as mothers”...

Dr. Kelly Brogan Wakes Up to the “Ball Earth Hoax”. What Does This Reveal About Prominent Professors From Prominent Medical Schools?
What did I mean when I said Dr. Kelly Brogan "won the pandemic"?
The Menace of Wellness Influencers
Wellness influencers are often also conspiracy theorists, as both mindsets rely upon the same underlying methods, motivation, and narrative.






Don’t Blame the Patient