Why antivax arguments for COVID-19 vaccine “shedding” remind me of homeopathy
An antivaxxer by the 'nym "A Midwestern Doctor" makes an argument that COVID-19 vaccine "shedding" is not impossible despite the basic science that concludes it is. Sound familiar?

A good journal breaks bad: AAP spreads misinformation about glyphosate
The latest report from the American Academy of Pediatrics is filled with misinformation and missing key articles that support the well-researched conclusion that there is no legitimate evidence of negative health effects of glyphosate.

Skeptics in the Pub. Cholera. Chapter 7b
Will this ever end? Eventually.

Dr. Lucy McBride: “As physicians, dispensing false hope is dangerous & unethical.”
The many sheltered physicians like Dr. Lucy McBride who confidently said herd immunity was at hand and fear of COVID was pathological are the last people who should be sanctimoniously sermonizing about the importance of trust in medicine.
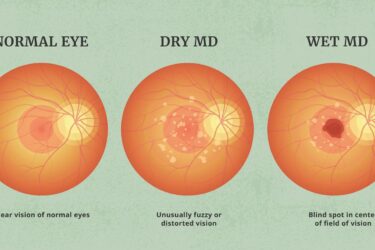
Pegcetacoplan (Syfovre™) for macular degeneration: an update
SBM's guest contributor and ophthalmologist, Dr. David Weinberg, provides an update on the phase 3 trials of pegcetacoplan for macular degeneration. The results are still disappointing.
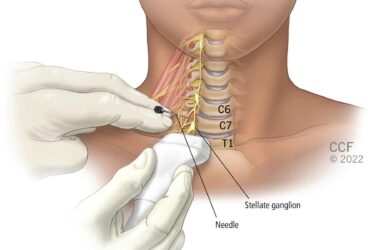
Dual Sympathetic Reset for PTSD
Dual Sympathetic Reset is being promoted as a treatment for PTSD prior to any convincing clinical evidence.

The Wellness Company: How antivaccine grift becomes plain old quackery
The Wellness Company, promoted by Dr. Peter McCullough, is the product of a trend in which antivax doctors have predictably become just quacks. At least in this case, there is an amusing quack fight at the heart of it all.

Skeptics in the Pub. Cholera. Chapter 7a
The story continues apace.

A Bit of Good News: Kids Appear to Have Lower Risk of Post-COVID Conditions Than Previously Thought
Based on a recently published study using improved criteria for determining long term COVID-related health problems, it looks like kids are less likely to be negatively impacted than previously thought.

2024 Detox Trends To Watch (Out) For
Trends come and go but the popularity of detoxification and cleansing in January is eternal.






Don’t Blame the Patient