Tag: acupuncture

Science-based medicine isn’t just for CAM. The case of ivermectin shows that it never was.
Another large randomized controlled trial for ivermectin showed no efficacy for the early treatment of COVID-19. This is not a surprise to science-based medicine advocates. Here's why the story of ivermectin shows that SBM isn't just for "complementary and alternative medicine" (CAM) —and never was.

Ivermectin: The acupuncture of COVID-19 treatments
As high-quality evidence increasingly and resoundingly shows that ivermectin does not work against COVID-19, advocates are doing what acupuncture advocates do: Turning to lower quality "positive" studies to claim incorrectly that their favorite ineffective treatment actually does "work".

Does Acupuncture Increase Red and White Blood Cells and T-Cells?
An article by a medical acupuncturist claims that acupuncture increases red and white blood cells and T-cells. The evidence is far from convincing.

Even in a pandemic, bait-and-switch acupuncture studies still get published in Nature
Last week, a study claiming to have identified a neurologic mechanism by which acupuncture reduces inflammation was published in Nature. It does no such thing. it's another bait-and-switch mouse study that likely would never have been published in such a high profile journal if it hadn't rebranded electrical stimulation as "electroacupuncture".
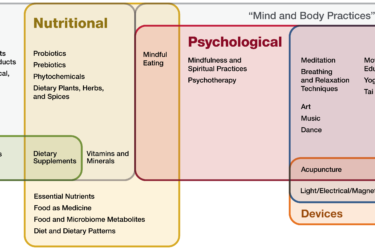
NCCIH Strategic Plan 2021–2025: Meet the new plan, same as the old plan…?
The National Center for Complementary and Integrative Health recently released its latest 5 year strategic plan. It's basically the same as the last strategic plan, but with one new addition. It's not really a new addition, but it signals a resurrection of an old trope about "integrating" quackery with science-based medicine.
Catgut Acupuncture
Catgut acupuncture is but one example of how acupuncture's basis in pseudoscience provides an infinitely malleable template for fabricated mechanisms of action and feigned health benefits.
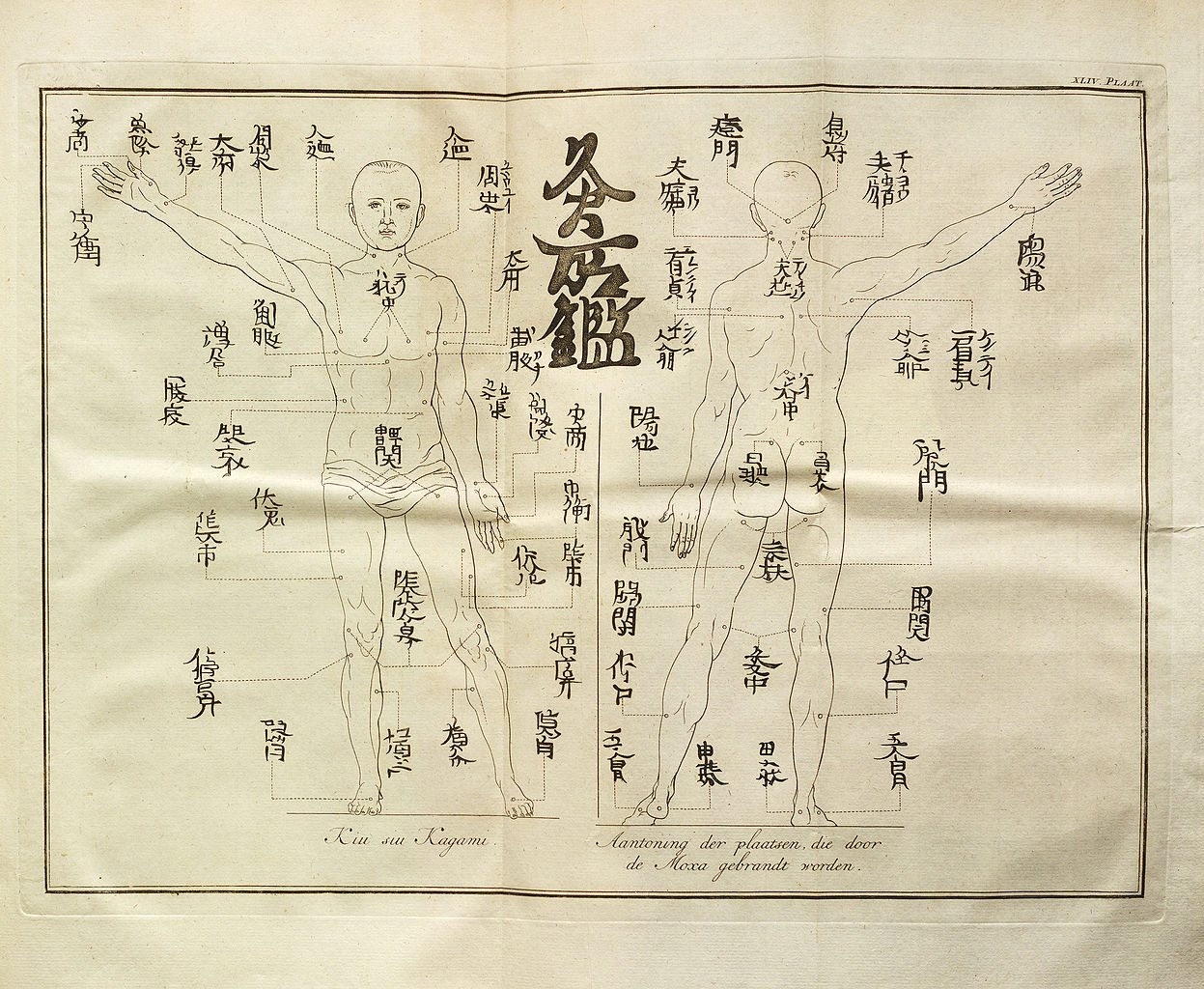
A Worthless Acupuncture Study in Cancer Patients
This study does not test the efficacy of acupuncture and was never designed to do so.
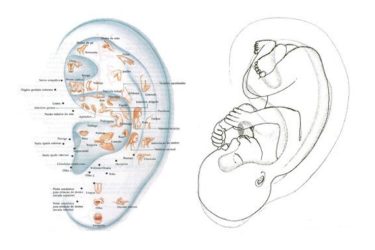
Ear Acupuncture for Procedural Pain in Neonates: More Randomized Controlled Nonsense
A recently published multicenter randomized and placebo controlled study attempted to answer the question of whether or not magnetic acupuncture beads stuck on premature baby ears reduced pain during a common screening exam. They don't. And they might have made things worse for these babies.

Aroma Acupoint Therapy
"Aroma acupoint therapy" demonstrates how the combination of several nonsensical ideas involving essential oils and acupuncture produces, unsurprisingly, yet another nonsensical CAM treatment.


