Tag: pediatrics

A good journal breaks bad: AAP spreads misinformation about glyphosate
The latest report from the American Academy of Pediatrics is filled with misinformation and missing key articles that support the well-researched conclusion that there is no legitimate evidence of negative health effects of glyphosate.
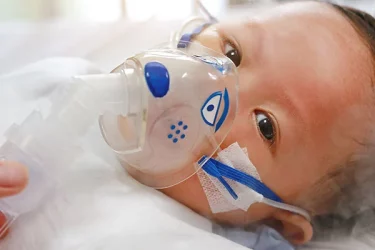
The 2022-2023 Respiratory Virus Season Hits Early and Hard: Part 2
What is RSV and why is it so bad this season? I discuss this and a promising new vaccine candidate.

Letter to a Medical Student: You Erred. You Are Owed an Apology.
While you are an adult who is responsible for your own words, the editors of Sensible Medicine did you a grave disservice by letting you publish your article.

A Popular Home Remedy Causes Severe Burns in Pediatric Patients
Garlic has been used medicinally for thousands of years, but the evidence for benefit isn't great. And topical use, particularly in young children, can cause severe burns. Stick to using garlic as a recipe ingredient rather than as a remedy.

Impressive New Data on the Benefit of Childhood Vaccines
A new study adds compelling evidence that vaccines given to young children prevents disease and saves the lives of people of all ages. It may not be surprising, but it's nice to see. Spread the word.
CDC Issues Warning as the Virus Associated with a Rare Polio-Like Illness in Children Returns
After a pandemic related lull, pediatric respiratory infections are roaring back. Unfortunately, this means that there will likely be a spike in cases of a polio-like illness caused by enterovirus D68.
The Alternative to Vaccinating Children Isn’t Just “Not Vaccinating” Them
It's putting them on an inevitable collision course with the virus—without any protection from the vaccine.
COVID-19 vaccination and myocarditis: another preprint
A preprint from Thailand gives us more information about vaccine-associated myocarditis in younger people, but should not be weaponized by antivaccine activists as a reason to avoid vaccination against COVID-19.

“Natural Immunity” Stans Forget Babies Will Always be Vulnerable to COVID
Children are still getting hospitalized with COVID, no matter how many times contrarian doctors mindlessly repeat the mantra "natural immunity". Doctors who know where babies come from understand why this might be.

Minimizing COVID Via Postmodernism
An exploration of how, under the guise of "reason", doctors who desperate to be different no matter the evidence have embraced the position that there are no aspects of reality that are objective and that feelings matter more than facts.

