Year: 2013
Comprehending the Incomprehensible
Medicine is impossible. Really. The amount of information that flows out the interwebs is amazing and the time to absorb it is comparatively tiny. If you work, sleep and have a family, once those responsibilities are complete there is remarkably little time to keep up with the primary literature. I have made two of my hobbies (blogging and podcasting) dovetail with my...
At Your Own Risk
In 2011, Americans spent some $30 billion on dietary supplements. Yet, except for the industry itself and a few politicians and “health freedom” advocates, you’d be hard pressed to find anyone (who’s given it some thought) of the opinion that dietary supplement regulation is adequate. Three recent reports, two from the government and one from a newspaper, demonstrate why this near-universal conclusion...
Clinical Decision-Making Part III
How do doctors make clinical decisions to arrive at a diagnosis? Part 3 of a 3-part series.
Dr. Amen’s Love Affair with SPECT Scans
Daniel Amen loves SPECT scans (Single Photon Emission Computed Tomography). And well he should. They have brought him fame and fortune. They have rewarded him with a chain of Amen Clinics, a presence on PBS, lucrative speaking engagements, a $4.8 million mansion overlooking the Pacific Ocean, and a line of products including books, videos and diet supplements (“nutraceuticals”). He grossed $20 million...
It’s a part of my paleo fantasy, it’s a part of my paleo dream
There are many fallacies that undergird alternative medicine, which evolved into “complementary and alternative medicine” (CAM), and for which the preferred term among its advocates is now “integrative medicine,” meant to imply the “best of both worlds.” If I had to pick one fallacy that rules above all among proponents of CAM/IM, it would have to be either the naturalistic fallacy (i.e.,...
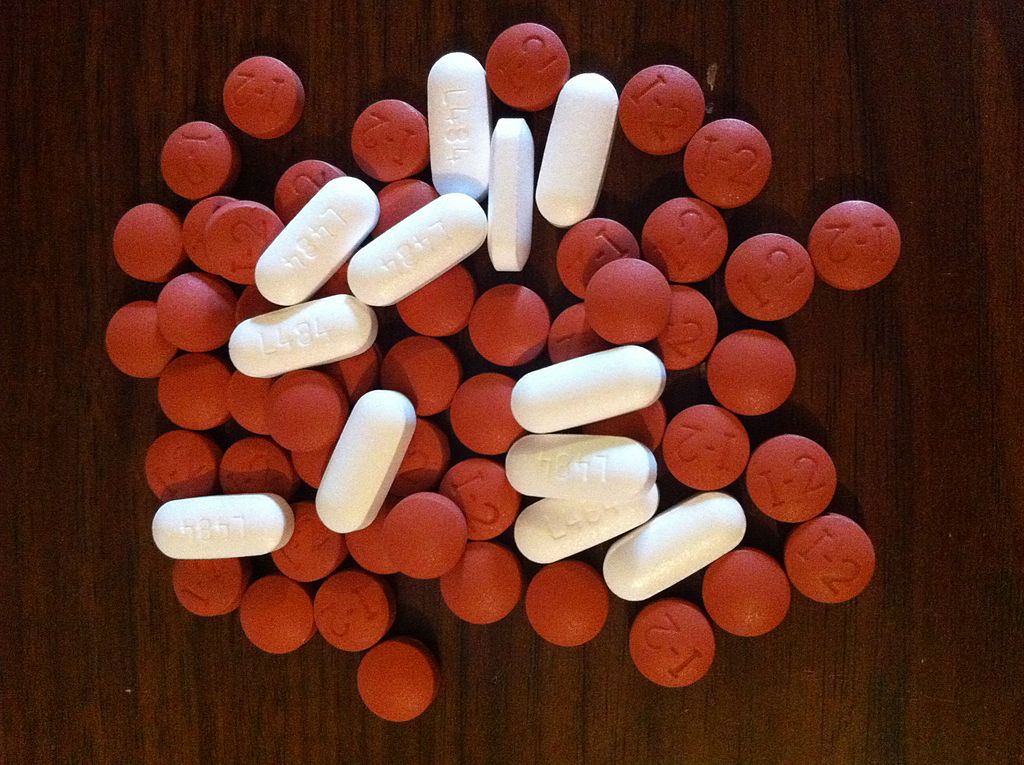
Anti-inflammatory drugs: A closer look at the risks
If science-based medicine reflects the application of the best evidence, then we should expect practices to change when new data emerges. In the long run that’s generally true, and the progressive gains we’ve seen in the management of disease reflect this. But in the short run, change can be maddeningly slow, and there are many areas of medicine where we could be...
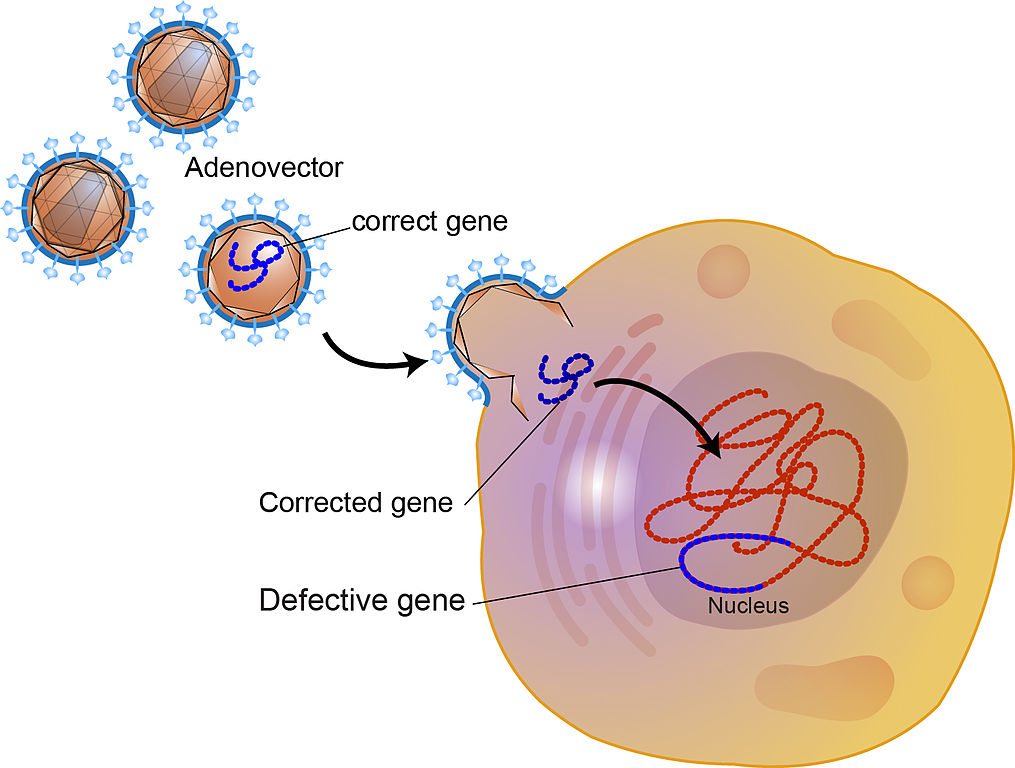
Burzynski: Cancer Is A Serious Business, Part 2: Like the first Burzynski movie, only more so?
Film producer Eric Merola seems to think that there is a conspiracy of skeptics (whom he calls The Skeptics) who are fanatically hell-bent on harassing his hero, Brave Maverick Doctor Stanislaw Burzynski. According to his latest film Burzynski: Cancer Is A Serious Business, Part 2 (henceforth referred to as Burzynski II, to distinguish it from part 1, to which I will refer...

Clinical Decision-Making: Part II
How do doctors make clinical decisions to arrive at a diagnosis? Part 2 of a 3-part series.
Smoking: The Good News and the Bad News
The principles we espouse on Science-Based Medicine are vitally important, but some of the subjects we address are not so important in the big scheme of things. Homeopathy and electrodermal diagnostic devices don’t actually harm very many people. For today’s post, I’m going to follow the Willie Sutton rule and go where the money is, so to speak. Smoking is the leading preventable...
Three myths about Stanislaw Burzynski and The Skeptics
As I finished last week’s post, I promised myself that I wouldn’t write about Stanislaw Burzynski again this week. After all, counting this post I will have done 13 posts so far in 2013, and, counting this one, four of them will have been about Burzynski, and three out of the last five posts (three out of four, really, if we eliminate...

