Year: 2013
Acupuncture and Allergic Rhinitis: Another Opportunity for Intellectual Sterility
You need to keep an open mind. A common suggestion offered to naysayers of nonsense. The usual retort concerns not letting one’s brain fall out. Evaluating SCAM’s is less about having an open mind and more about having standards, a conceptual framework that is used to interpret and analyze new information. One of the benefits of writing and reading topics covered by...
Legislative Alchemy: Acupuncture and Homeopathy 2013
Acupuncture, or more broadly, Oriental or Traditional Chinese Medicine, is a weird medley of philosophy, religion, superstition, magic, alchemy, astrology, feng shui, divination, sorcery, demonology and quackery. And via the particular form of magic known as legislative alchemy, acupuncture is a licensed health care profession in 44 states and the District of Columbia. A growing body of evidence demonstrates acupuncture is simply...
Time for a little blatant self-promotion
I thought I’d take advantage of my prerogative as managing editor of this blog to do a quick bit of blatant self-promotion. I will be in the Washington, DC area later this week, and while I’m there to attend the Society of Surgical Oncology Annual Cancer Symposium, I’ll also be taking advantage to do a little side trip to give a talk...
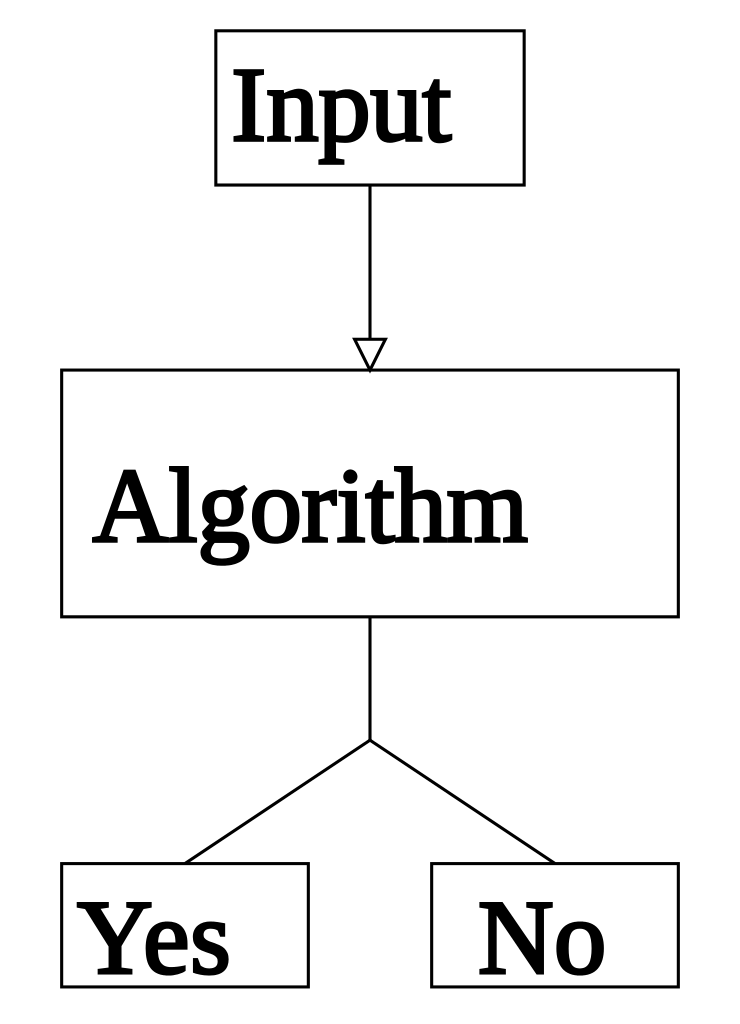
Clinical Decision Making: Part I
How do doctors make clinical decisions to arrive at a diagnosis? Part 1 of a 3-part series.
Bogus Electrodermal Testing Devices and the Failure of Regulators to Act
Electrodermal testing is a bogus procedure where measurements of skin conductance with a biofeedback device are entered into a computer to diagnose nonexistent health problems and “energy imbalances” and to recommend treatments for them, often involving the sale of homeopathic remedies and other useless products. It falls under the general category of EAV (Electro Acupuncture of Voll). The history and variants of...
Dr. Stanislaw Burzynski’s cancer “success” stories update: Why is the release of the Burzynski sequel being delayed?
It’s no secret that I happen to be on several mailing lists of groups or doctors whose dedication to science is—shall we say?—questionable. Of course, the reason I join such mailing lists is to keep my finger on the pulse of pseudoscience, so to speak. Between such lists and strategically selected Google Alerts (the latter of which appear to be failing me...
Chiropractic and Sudden Infant Death Syndrome
As a pediatrician caring for hospitalized children, I deal with fear on a daily basis. My day is saturated with it. I encounter fear in a variety of presentations, with parental fear the most obvious but probably least impactful on my management decisions. I do spend a lot of time and mental energy calming the fears of others but more managing my...
Calcium supplements and heart attacks: More data, more questions
Why take a drug, herb or any other supplement? It’s usually because we believe the substance will do something desirable, and that we’re doing more good than harm. To be truly rational we’d carefully evaluate the expected risks and benefits, estimate the overall odds of a good outcome, and then make a decision that would weigh these factors against any costs (if...
Doctors and Dying
“I intend to live forever. So far, so good.” – Steven Wright The humor in many of comedian Steven Wright’s famous one-liners is that they are simultaneously familiar and absurd. At some level we all know that we are going to die, but as long as we are still alive (or a loved-one is alive) we can cling to the irrational hope,...
Kudos to a Journalist
Many SBM readers will remember the late, great Barry Beyerstein, a luminary of the skeptical movement and author of a classic article that has been cited many times on SBM, an explanation of why bogus therapies seem to work. One of his greatest personal accomplishments is not as well known: he produced an exceptional daughter, Lindsay Beyerstein, a freelance writer, philosopher, and...

