
Motivation to Exercise in Mice
A new study in mice shows a connection between gut microbiome and willingness to exercise. Could this discovery lead to improved motivation to exercise in humans? Possibly, but we don't yet know if humans share the same pathway.

Quack Quack
Joe Schwarcz's new book Quack Quack is an informative and entertaining look at quackery and pseudoscience past and present. A delightful read.

Should You Take Vitamin D Supplements?
Recent research found that supplemental vitamin D doesn't prevent fractures or have any effect on the diseases it has been claimed to help, and blood tests for vitamin D are useless.

Treating Nightmares with a Smart Watch
Preliminary evidence suggests a watch may help people with severe nightmares. Of course, more research is needed.

Is Meat Poison? Is Fat the Antidote?
Is a diet comprised solely of meat good for you? I think you know the answer.

Balm of Gilead
Balm of Gilead was mentioned in the Bible, but we don't know what was in it. It is supposed to relieve pain, but we don't know if it is effective; there are no controlled studies.

GOLO for Weight Loss
There are lots of testimonials from people who say they lost weight with GOLO, but its effectiveness is not supported by any scientific evidence.
In Through the Nose, Out Through the Mouth
The advice to breathe "in through the nose, out through the mouth" appears to be based on superstition rather than science. Nose breathing is preferable.
Medicare and Alternative Medicine
Medicare is paying for nonsense.
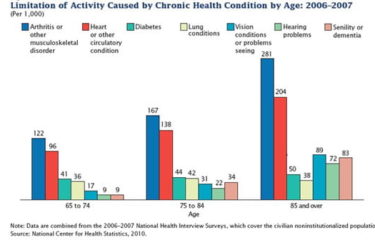
Geriatric Preventive Medicine Appointments Covered by Medicare
Medicare offers free preventive medicine visits for those over 65: the Welcome to Medicare visit and the Annual Wellness Visit. Increased awareness of these benefits would improve health care, save taxpayer money, and reduce inequities of preventive medicine care for underserved populations.

