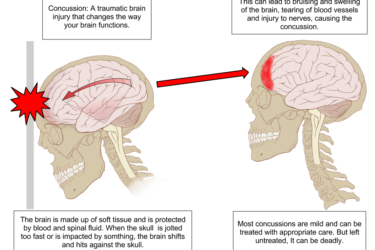
Chiropractor Treating Concussions for Earlier Return to Play
A chiropractor is using questionable diagnostic and therapeutic measures to return athletes to play sooner after a concussion. Not a good idea.
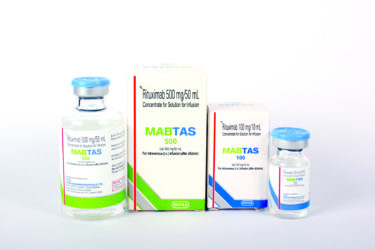
Chronic Fatigue Syndrome and Rituximab
IV rituximab has been used to treat chronic fatigue syndrome. A large, well-designed new study shows it doesn't work.

Medical Apartheid
Harriet Washington's book tells the dark history of medical experimentation on black Americans. It also reveals broader problems of inequality, poor science, and human failures.

Great Courses: Skeptic’s Guide to Health, Medicine, and the Media
Dr. Roy Benaroch's course offers a toolkit of six questions we can use to evaluate the truth behind the often misleading media reports on health topics. It is a valuable companion to the Science-Based Medicine blog.

For Discussion: Should I Only Write About Fake Stuff If It Is Well-Known?
Does writing about questionable topics that are not well-known do more harm or good? There are arguments on both sides.

The “Evidence” for Prodovite Is Junk Science
Prodovite is a liquid nutritional supplement marketed as "nutrition you can feel." The claims are pseudoscientific nonsense and the single unblinded clinical study is junk science that relies on a bogus test: live cell microscopy.
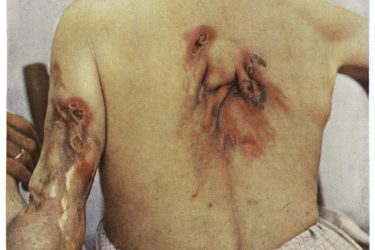
The Tuskegee Syphilis Experiment: A Fiasco with a Silver Lining
The Tuskegee syphilis experiment studied black men with advanced syphilis for 40 years. Patients were lied to and prevented from getting treatment. A black mark in the history of American medicine, it led to important reforms.

Homeopath Quits Homeopathy but Thinks the Homeopathic Approach Has Value
A former homeopath shows that there's nothing scientific about homeopathy; in fact, it contradicts all known scientific principles. Nevertheless she finds value in the homeopathic approach to the patient and thinks all providers can learn from it.



