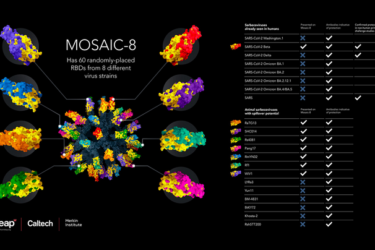
Possible Universal Coronavirus Vaccine
New research potentially points the way to a universal coronavirus vaccine and other applications.
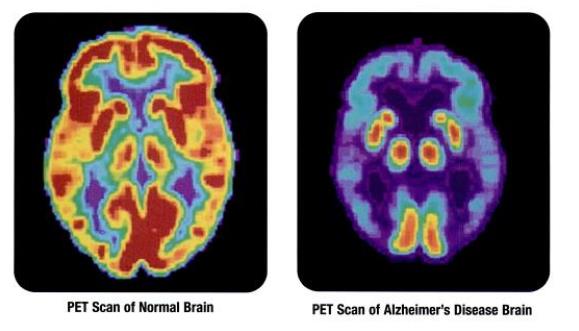
COVID Associated With Neurodegenerative Disorders
COVID infection has been associated with an increased risk of neurodegenerative and neurovascular disease - another reason to keep our eye on this serious illness.

US Preventive Services Task Force Recommends Against Multivitamins
An updated review of the evidence reinforces that routine vitamin use is mostly worthless.

How Safe is CBD?
CBD is a drug, but sold as both a drug and herbal supplement. What does the current evidence say about its safety?

Is There a Replication Crisis?
The true causes and implications of the replication problem in science.

Black Market Anti-virals
New antivirals for COVID have rapidly led to a black market in dubious knock-offs.
Should We Fear the Monkeypox?
A recent outbreak of monkeypox is likely containable, but people are understandably concerned.
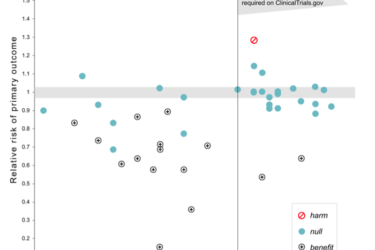
Homeopathy and Pre-Registered Trials
Preregistering clinical trials is a great idea, but we have to actually track registration.
The Toll of COVID
We can't take our eyes off the ball just yet - what's the state of the pandemic?


Sex and Racial Bias in Cardiac Care
Sex and racial biases in cardiac care partly reflect cognitive biases that can be corrected with education.