
Pesticide in Oat Products – Should You Worry?
You know the rule about headlines - if there is a question in a headline the answer is almost always "no". This article is no exception.

Mayo Clinic Promotes Reiki
The Mayo Clinic is a prestigious medical institution with a deserved international reputation. It also promotes rank pseudoscience. It does this, apparently, for all the reasons we have explored here at SBM over the years. I have seen first hand how one or a few true believers can promote so-called alternative medicine at their institutions, meeting little resistance from colleagues and administrators...
The Menace of Wellness Influencers
Wellness influencers are often also conspiracy theorists, as both mindsets rely upon the same underlying methods, motivation, and narrative.

Adulteration of Herbal Supplements Continues
The supplement industry continues to be plagued by deliberate adulteration of products.
Cameroon Begins First Malaria Vaccine Program
Despite massive efforts to reduce the disease burden of malaria, it remains a significant cause of disease and death in parts of the world, most notably Sub-Saharan Africa. Now we have a new tool in the fight against malaria – two safe and effective vaccines. Cameroon is just beginning a program to give the vaccine for free to children in four doses...
Hospital Measures Prevented COVID Transmission
A new study finds that hospital measures to limit the spread of COVID-19 worked, and we probably should keep them.
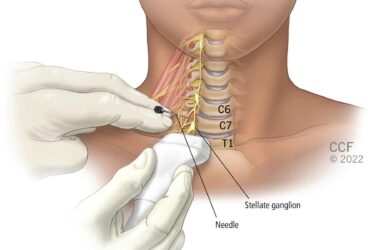
Dual Sympathetic Reset for PTSD
Dual Sympathetic Reset is being promoted as a treatment for PTSD prior to any convincing clinical evidence.
Medical Science in 2024
What medical breakthrough are likely in the near future?

SBM in 2023
Some thoughts as we complete our 15th year of science-based medicine.


What Is Somatic Therapy?
Is modern medicine descending into pseudoscience, or is scientific medicine still going strong? Unfortunately, I think both of these things can happen at the same time. On the one hand, scientific research in medicine is progressing nicely. We are seeing the results of scientific breakthroughs made decades ago, with monoclonal antibody therapies, new therapeutic targets, the beginning of real genetic therapy, brain-machine...