
Study on Acupuncture for Angina
Another acupuncture study claims positive results, but is plagued by methodological flaws and dubious results.
The Latest Ebola Outbreak
The second largest Ebola outbreak is underway. This time we have an effective vaccine, but political unrest and distrust of science may be our real vulnerability.

France To End Reimbursement for Homeopathy
Setback for homeopathy in France as a government agency actually does its job, but the fight against pseudoscience is long from over.
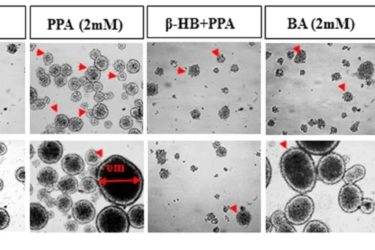
Processed Foods and Autism
Reports of a "link" between processed food and autism highly misrepresent the actual findings of an in-vitro study.

Media Literacy Is Key
Media literacy is an important component to teaching science and critical thinking. We'll add that to our to-do list.

Radioactive Energy Cards
Thailand officials warn of a radioactive snake-oil "energy card." It's worse than worthless – it's actively dangerous.

Taking On the Wellness Industry
The wellness industry is just one more manifestation of quackery and pseudoscience in health.

WHO Promotes Unscientific TCM
The World Health Organization endorses quackery in the form of TCM.

Time to Move Beyond the Impact Factor
The impact factor has become the one metric for journal quality. It's time to rethink this system.


Shaping Opinions About Science and Medicine
Responding to a commentary with all the usual anti-science tropes.