
Coca-Cola and Corporate Sponsored Research
A new study reveals that Coca-Cola included restrictive clauses in some research funding contracts. This is a good opportunity to review how such behavior can be stopped.
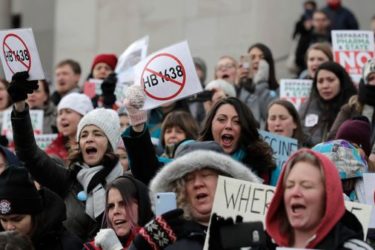
How To Respond to Anti-Vaxxers
How do we best address the anti-vaccine phenomenon? It's complicated.

Debunking Sleep Myths
Dispelling common sleep myths is the first step to improving one's sleep.

Another Measles Outbreak – Blame Antivaxxers
We are in the midst of record-breaking measles outbreaks. This is the time to push for stronger regulations and to get rid of non-medical exemptions.

Update on Glyphosate
A legal decision against the makers of glyphosate is not supported by the science.
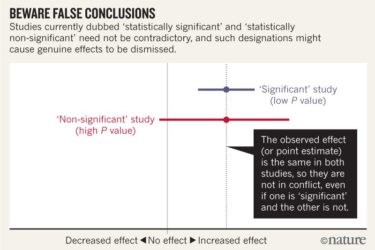
Statistical Significance and Toxicity
Researchers propose to get rid of the use statistical significance in science reporting. The idea has merit.

Fighting Online for SBM
Physicians are being harassed offline by antivax and other trolls. We can't let that happen.

Scientists Sign Petition Warning about EMF
A petition signed by 250 scientists warns about wireless technology, but the science is not on their side.

Canada Is Sending Homeopaths to Honduras
The Canadian government is sending homeopaths to Honduras as part of an aid program. They dropped the ball on this one, and should just admit error and correct it, but they are doubling-down instead.


JAMA on Medical Misinformation
A JAMA article addresses the issue of confronting medical misinformation. They make good recommendations - but do not go nearly far enough.