
Release Active Drugs – Homeopathy By Another Name
A Russian company is marketing "release active drugs" as a new medical technology, but it is just bogus homeopathy dressed up with new jargon.

Chinese Researcher Reports First Gene-Edited Babies
A Chinese scientist announces first gene-edited babies, setting off a discussion of the science and ethics of using CRISPR on humans.
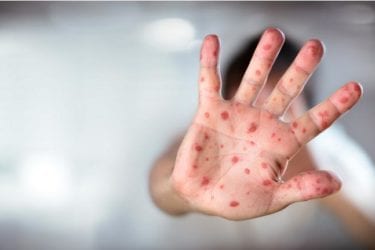
The Revenge of Chicken Pox
Another outbreak, this time chickenpox, can be blamed on antivaxxers.

Why People Deny Science
A new study further shows that people are inconsistent in how they justify their beliefs.
Update on Low Calorie Sweeteners
An updated review of the science finds that artificial sweeteners are still a safe and effective option for weight management.
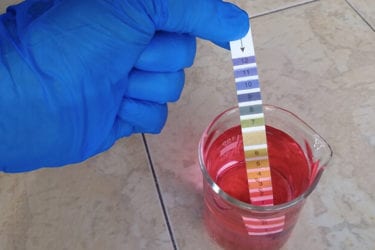
Alkaline Water Surges Despite Lack of Evidence
Alkaline water is pure BS – there is no plausibility to the claims of any health benefits, and what evidence we have is negative. Its popularity grows despite this.

Air Dryers vs Paper Towels
Which hand drying method is the best, air or paper towel? The answer is more complicated than you might think – but do wash your hands.
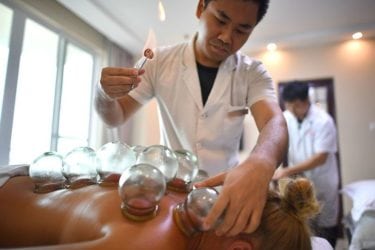
World Health Organization Endorses Quackery
The World Health Organization fails its primary function by promoting traditional quackery.

A Nuanced View on Breast vs Formula
While there is strong evidence that breast is best, a new study suggests that the benefits have been overstated, and may be mostly due to non-specific factors such as better education and overall health care.


Italy’s Antivaccine Government – The Attack on Experts Continues
Anti-vaccine Italian government fires its entire Health Council. This is unfortunately part of a bigger trend against expertise and reality-based policy.