Category: Chiropractic

The American Chiropractic Association Answers Crislip’s Call, Joins the Choosing Wisely Campaign
The Choosing Wisely campaign has invited the largest chiropractic organization in the United States to publish a list of interventions to avoid. The results, while not entirely without merit, consist of redundant or unnecessary recommendations. And there is a glaring absence of recommendations to avoid any of the blatant pseudoscience commonly practiced by chiropractors.

Chiropractor Disregards the Loss of His License, Continues to Treat Patients with Cervical Dysplasia with Escharotics
A chiropractor who bills himself as a chiropractic gynecologist has continued to practice after his license was permanently revoked. Among his many questionable practices, Nick LeRoy is treating cervical dysplasia with escharotics, a potentially dangerous replacement for conventional treatments to prevent cancer.

Yet Another Miscellany of Medical Malarkey
Acupuncture for menstrual cramps, chiropractic for the prevention of domestic terrorism, and more in this miscellany of medical malarkey. Or would you prefer hodgepodge of healthcare hokum?

Maximized Living: “5 Essentials” of Chiropractic Marketing Propaganda
What do vitalism, old school chiropractic subluxations, germ theory denial, detox supplements, marketing gimmicks, and practicing way beyond a reasonable scope have in common?
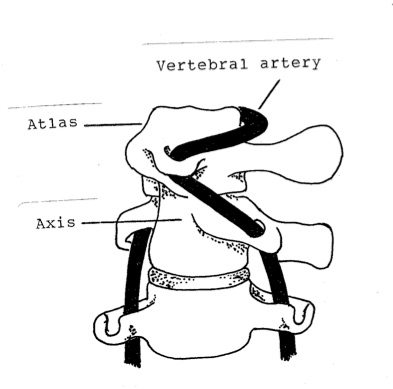
Study: patients should be warned of stroke risk before chiropractic neck manipulation
Another study adds to growing body of evidence that chiropractic neck manipulation is a risk factor for stroke. Patients should be warned of risk.
Science-Based Satire: Australian Fetus First to Undergo Intrauterine Chiropractic Adjustment
Are chiropractic surgeons really performing intrauterine spinal adjustments based on the results of nonsensical muscle tests and ultrasound imaging? No.

Chiropractic and Spinal Manipulation Red Flags: A Comprehensive Review
Many people visit chiropractors’ offices seeking relief from back pain. Appropriate use of spinal manipulation provided by a chiropractor can be helpful in treating mechanical-type back pain, but there are good reasons to avoid chiropractic manipulation based on correction of “vertebral subluxations,” and there are red flags to look for before undergoing any kind of manipulative treatment for neck or back pain.
Chiropractic clinical training with pediatric patients or complicated cases: slim to none
Chiropractors may never have seen a pediatric patient or a complicated medical case in clinical training, yet they are allowed to go into practice with no age limits on who they see and few on the conditions they treat.