Category: Epidemiology
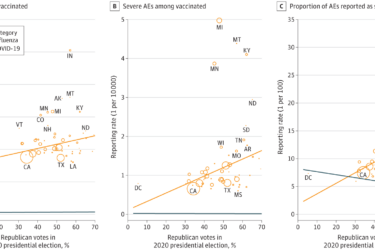
Dr. Vinay Prasad vs. a VAERS study finding more reports of vaccine injury in red states
Dr. Vinay Prasad attacks an epidemiological study published in JAMA Open Network reporting that people in red states are more likely to report vaccine injuries, claiming that a more rigorous study would "not be difficult," when he knows that it would be very difficult.

How antivaxxers weaponize vaccine safety studies to falsely portray vaccines as dangerous
Antivaxxers have weaponized a huge multinational vaccine safety study of 99 million patient records that found rare adverse events and concluded that the risks of COVID-19 vaccines outweigh the benefits. How? A combination of the Nirvana fallacy and spin.

He pushed hydroxychloroquine three years ago: Harvey Risch and false claim of “turbo cancers” caused by COVID-19 vaccines
Last week, I discussed Dr. William Makis' false claims of "turbo cancers" due to COVID-19 vaccines. Now it's hydroxychloroquine-promoting epidemiologist Harvey Risch's turn.

Autism prevalence increases to 1 in 38, and antivaxxers blame vaccines without using the word “vaccine”
The CDC updated its estimates for the prevalence of autism spectrum disorders. Predictably, antivaxxers blame the increasing prevalence of ASDs reported, particularly in Black children, on "environmental factors," which is antivax code for, "Vaccines are to blame."
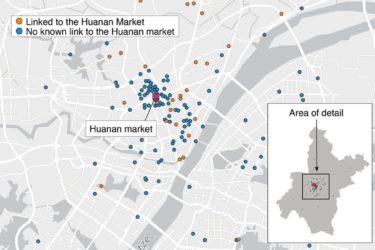
The rise and fall of the lab leak hypothesis for the origin of SARS-CoV-2
Two new studies were published last week that strongly support a natural zoonotic origin for COVID-19 centered at the wet market in Wuhan, China. Naturally, lab leak proponents soberly considered this new evidence and thought about changing their minds. Just kidding! They doubled down on the conspiracy mongering, because of course they did.

Antivaxxers misuse the Defense Medical Epidemiology Database to demonize COVID-19 vaccines
Over the last couple of weeks, a claim that the Defense Medical Epidemiology Database (DMED) shows that COVID-19 vaccines have caused a massive increase in cancer, neurological, and cardiovascular diseases in military personnel has gone viral. A closer look shows that the increases are almost certainly spurious and due to underreporting in previous years.

The dumpster diving VAERS preprint debacle: How did we get here?
Last week, SBM devoted a lot of digital ink to a poorly done study analyzing the VAERS database for myocarditis after COVID-19 vaccination that was widely publicized to imply that the vaccine is more dangerous than the disease. Three out of the four authors should have known better, leading me to ask: How did we get here?

Dumpster diving in the VAERS database to find more COVID-19 vaccine-associated myocarditis in children
"Dumpster diving" is a term used to describe studies using data from the Vaccine Adverse Events Reporting System database by authors, almost always antivaxxers, who don't understand its limitations. Last week, non-antivax doctors who should know better fell into this trap when they promoted their study suggesting that COVID-19 mRNA vaccines are more dangerous to children than the disease.