Category: Herbs & Supplements

Billions on herbal remedies – and for what?
Consumers spend billions each year on herbal remedies, with little to show for it.
Alkaline Water Surges Despite Lack of Evidence
Alkaline water is pure BS – there is no plausibility to the claims of any health benefits, and what evidence we have is negative. Its popularity grows despite this.

Gold Water, Silver Water, Copper Water
Ayurveda recommends gold water, silver water, and copper water to treat various conditions. There is no evidence that they work or even that they contain gold, silver, or copper.
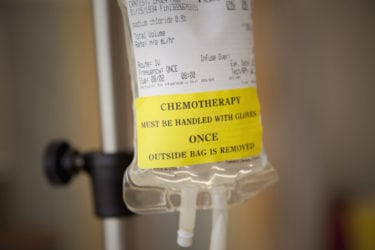
A whole issue of JACM devoted to “integrative oncology” propaganda? Oh, goody.
Last week, The Journal of Alternative and Complementary Medicine published a Special Focus Issue on "integrative oncology." In reality, it's propaganda that promotes pseudoscience and the "integration" of quackery into oncology.

Fish Oil Doesn’t Help Dry Eyes
Dry eyes? Despite guidelines that recommend fish oil consumption, a new trial demonstrate that they are not effective.
Integrative Medicine finally admits it’s attracting bad apples
Integrative medicine proponents finally acknowledge their field is attracting bad apples but fail to identify the real source of their problem: It's rejection of science-based medicine, not lack of training in integrative medicine.

Kratom – An Emerging Herbal Drug
Kratom is an emerging herbal drug used for pain and fatigue but also has abuse potential. What is the current state of the science?

Naturopathy Textbook
The Textbook of Natural Medicine reveals what students of naturopathy are taught. It claims to be a scientific presentation, but it reveals just how unscientific naturopathy is. It mixes good science with bad science, pseudoscience, outright errors of fact, vitalism, philosophy, ancient history, superstition, gullibility, misrepresentations, metaphysics, religion, hearsay, opinion, and anecdotes.

No Benefit from Fish Oil
A new systematic review of clinical trials shows no clear benefit to consuming omega-3 fatty acids in food or supplements.

FDA blacklists cesium chloride, ineffective and dangerous naturopathic cancer treatment
The FDA recently issued an alert warning of significant safety risks associated with cesium chloride. It is a mineral salt promoted by naturopathic “doctors” and “integrative” medicine practitioners as an alternative treatment for cancer, despite the lack of evidence of safety and efficacy in treating cancer or any other disease.

