Category: Neuroscience/Mental Health
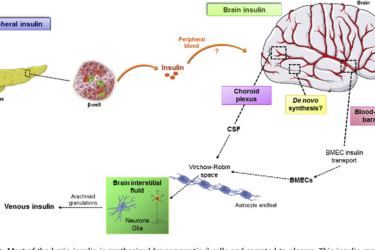
What Is Type 3 Diabetes?
I’m always wary of new medical terms that seem to be used and promoted prematurely, when still in the hypothesis phase. It seems like an obvious way to bias any thinking about an alleged phenomenon – just label it as the hypothesis, as if it is already a conclusion. Calling symptoms that may follow a lyme infection “chronic lyme disease” implies something...
“New school” antivax goes old school as Byram Bridle asks if COVID-19 vaccines will drive an “epidemic” of autism
Wakefield redux? Antivax scientist Byram Bridle just took the "new school" antivax movement old school by implying that COVID-19 vaccines might cause an "epidemic of autism." Everything old is new again, sort of.
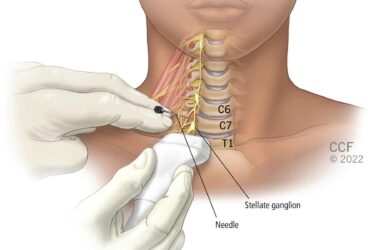
Dual Sympathetic Reset for PTSD
Dual Sympathetic Reset is being promoted as a treatment for PTSD prior to any convincing clinical evidence.

Cytotron – Magical Device Pseudoscience
The claims of Neurocytonix are extraordinary and dubious.

Internet Use and Mental Well-Being
Results of the largest study on internet use, well-being, and mental health.

FDA Approves Leqembi for Alzheimer’s
FDA upgrades Leqembi for AD from accelerated to traditional approval based on latest clinical data.

Dubious Autonomic Nervous System Claims
Beware overblown claims that autonomic testing can help almost anything.
What Is Dopamine Detox?
Just another fad that oversimplifies a complex problem to sell an easy fix.

Motivation to Exercise in Mice
A new study in mice shows a connection between gut microbiome and willingness to exercise. Could this discovery lead to improved motivation to exercise in humans? Possibly, but we don't yet know if humans share the same pathway.

Treating Nightmares with a Smart Watch
Preliminary evidence suggests a watch may help people with severe nightmares. Of course, more research is needed.

