Category: Public Health

The Scientific Integrity Act: Protecting science from politics
The proposed federal Scientific Integrity Act supports science and the scientific process as the basis of public policy and aims to protect it from politics, ideology, and financial conflicts of interest.

There’s No Vaccine for HIV/AIDS, But There’s Truvada
Science has made great strides in understanding, treating, and preventing HIV/AIDS. We can hope for an AIDS vaccine, but meanwhile there is a pill that can markedly reduce the risk of becoming infected.

Fat Shaming Is Counterproductive
Fat shaming not only doesn't work, it is counterproductive. So what might help fight obesity?

Soft Drinks and Death Risk
New study linking soft drinks to increased mortality is correlational only, and should be interpreted with caution.
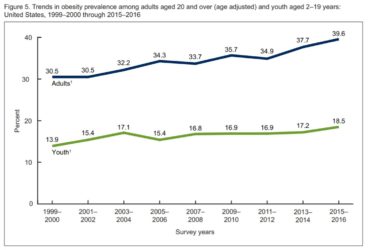
Update on the Obesity Epidemic
The obesity epidemic continues, and even accelerates, among continued debate about its causes and solutions.

Improving mental health is a walk in the park (but mind the volcanoes)
Using Twitter and geotagging, researchers add to the growing body of evidence demonstrating an association between contact with nature and improved mood.

Maternal Fluoride and IQ
New study purporting to show correlation between fluoride and IQ comes under heavy criticism.
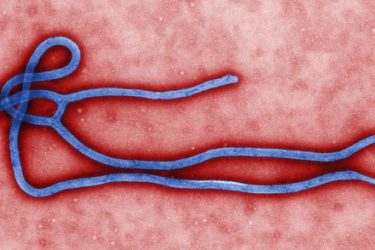
Ebola: Science Is Making Progress
Good news! Research on Ebola has identified a 100% effective vaccine and medications that produce a 90% survival rate.

Americans still (mostly) trust scientists and doctors, but there are some troubling warning signs
Given all the denial of the science behind vaccines, GMOs, evolution, and climate science, you might think that Americans in general distrust scientists and physicians. It's actually not true. Trust in scientists and doctors remains high, but there are still areas where mistrust of scientists is a significant problem. What can be done?


