Category: Public Health

The war on the science-based regulation of medicine accelerates
Last week, it was reported how increasingly there is a war on the science-based regulation of medicine and physicians. It's an old story, but unfortunately the forces arrayed against science-based policy have been emboldened by the pandemic and an stronger alliance with political groups that are against government regulation in general.
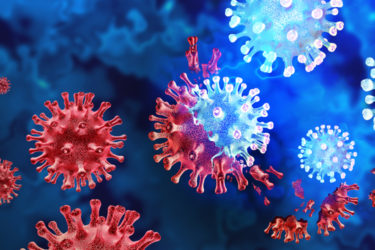
The Subvariants Are Coming
A wave of Omicron subvariants are coming. So get vaccinated.

Sleep Duration and Health
Poor sleep is a genuine concern, but the results of a new cohort study are complex to interpret.

Burden of Proof Studies and Health Risk
A new way of presenting knowledge about health risks highlights the ambiguity of the evidence and the importance of basic health behaviors.

The State of Florida spreads antivaccine disinformation disguised as an epidemiological “study”
On Friday, Florida State Surgeon General Dr. Joseph Ladapo released a non-peer-reviewed "study" that recommends against males aged 18 to 39 receiving mRNA COVID-19 vaccines based on bad epidemiology and science. This is the first time that we've seen a state government weaponize bad science to spread antivaccine disinformation as official policy, a dangerous new escalation in antivaccine propaganda.

“Censorship” and “thoughtcrime”? Antivaxxers and COVID-19 contrarians attack California AB 2098
One of the oldest tropes favored by quacks of all stripes, including antivaxxers, is to portray any attempt at regulating their quackery as an assault on freedom of speech. It's therefore not surprising that after its passage by the California legislature prominent spreaders of COVID-19 misinformation are labeling AB2098, which seeks clarify and codify the power of the Medical Board of California...

Healthcare Costs of Air Pollution
More recent estimates of the health related costs of air pollution are staggering.

PreP for HIV/AIDS
Two pills and an injection are FDA-approved to prevent HIV infection. Not enough patients and providers know about them.

COVID-19 vaccines and the Nuremberg Code
Antivaxxers love to claim that vaccine mandates (especially COVID-19 vaccine mandates) violate the Nuremberg Code and call for Nuremberg-style tribunals to hold public health and vaccine advocates "accountable". As usual, they have no idea what they are talking about. This is also not a new antivax narrative, although what is unprecedented is that what was once fringe even among antivaxxers is now...