Category: Science and Medicine

Every Time Dr. Jay Bhattacharya Talks About COVID, He Proves He Was Totally Wrong About COVID
Dr. Jay Bhattacharya March 2020: "If it’s true that the novel coronavirus would kill millions without shelter-in-place orders and quarantines, then the extraordinary measures being carried out in cities and states around the country are surely justified."

Skeptics in the Pub. Cholera. Chapter 15 minus 1
For those more observant than a semi-senile old man, I cut and pasted the wrong text this morning. Now updated. Good thing I am retired.

The Failed “We Want Them Infected” Movement Is Trying to Rebrand Itself As The “All We Really Wanted Was Poor Kids in School” Movement.
Part 2: In 2020, pro-infection doctors said "It’s fantastic news that we have a lot of cases." Today, they performatively lament "learning loss for children, especially in poor families". What happened to their assurances that the mass infection of unvaccinated youth will rapidly lead to herd immunity?

The Truth vs. Alex Jones: How the DSHEA of 1994 gave conspiracy mongers the means to fund their empires
As the HBO documentary The Truth vs. Alex Jones shows, Alex Jones promoted the conspiracy theory that the Sandy Hook massacre was a hoax to sell his supplement line. It's a model that many Internet conspiracy theorists use, like Mike Adams. Did the DSHEA help create Alex Jones and the modern conspiracy industry?

Dr. Marty Makary: “We’ll Have Herd Immunity by April” & “It’s Okay To Have an Incorrect Scientific Hypothesis. But When New Data Proves It Wrong, You Have To Adapt.”
Part 1: Doctors who said the pandemic ended 3-years ago now have the audacity to lament the "damaged public trust in the medical profession."
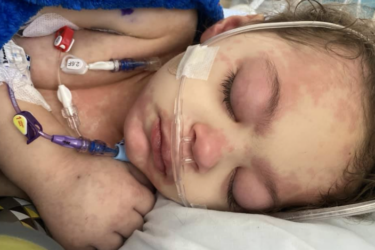
COVID-19 Vaccination Significantly Reduces Risk of Severe Inflammatory Syndrome in Kids
A new analysis of 2023 MIS-C cases reveals that the COVID-19 vaccine significantly reduces the risk of this dreaded complication.

AI for prescription drug information: Not yet useful for health care – but it’s coming
ChatGPT may not replace a health care professional's assessment yet, but its capabilities are growing.

Mark Sircus and “natural allopathic medicine”? Now I’ve heard everything from quacks
The term "allopathic medicine" was invented by homeopaths in the 19th century as a disparaging term for medicine. So to see a quack like Mark Sircus try to coopt it as "natural allopathic medicine" is quite something.

Some Doctors Cared Much More About Sore Arms Than Cold Bodies
The campaign against boosters was just a small part of a pathetic, pandemic-long pattern where doctors expressed grave concern about the mildest harms of measures to limit COVID, even purely theoretical ones, while being totally indifferent to literally anything the virus could do, including the deaths of children and young adults.

Best Hospital Eye Roll
Science: Figuring things out is better than making things up. A tee shirt I recently saw. Except… In a recent post Mayo Clinic Promotes Reiki, Steve seemed surprised that the Mayo was offering Reiki. I don’t know. Maybe he was channeling Louie. I know the Mayo is a top hospital, but I trained in Minneapolis at Hennepin County and we would have...

