Category: Science and Medicine

An Open Letter to ZDoggMD
I hope you'll agree with me that the biggest advocate for vaccination on social media should have no trouble sharing all of the facts about COVID-19 and children on a very frequent basis.

Medicare and Medicaid place restrictions on new Alzheimer’s drug, Aduhelm (aducanumab)
An important decision has been made about a controversial new drug to treat Alzheimer's disease.

A Modest Proposal: Schools Must Open With Untested, Unmasked, Unvaccinated Children
Kids don’t need Covid-19 vaccines to return to school and the downsides of masking young students are real.

Substack: Where quacks and antivaxxers all go now
With social media companies like Twitter and Facebook/Meta deplatforming those spreading misinformation, COVID-19 quacks, antivaxxers, and conspiracy theorists are flocking to Substack, where they can monetize their misinformation while Substack profits.

Everything old is new again
Since the pandemic hit, I've frequently said things like, "Everything old is new again", referring to the antivaccine movement in the age of COVID-19. As 2022 dawned, I thought I'd expand a bit on what I mean. Is there a term for déjà vu, but what I'm seeing now is amplified a thousand-fold? Proponents of science-based medicine have been warning us for...

Bioptron: Too Silly to Write about
Bioptron is a silly device claiming to work through unproven means, but basically seems to be an extremely colorful flashlight.
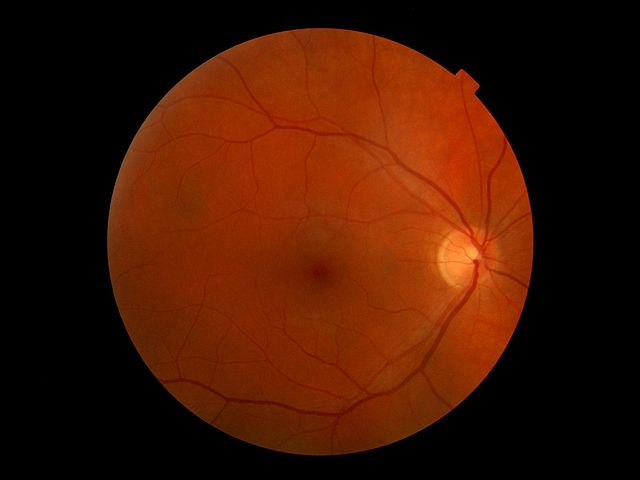
The Stem Cell Ophthalmology Treatment Study
In this study we have 300 patients with 47 different diseases subject to 7 experimental treatments among 3 treatment groups and no control group. What could possibly go right?




