Category: Science and Medicine

Maximized Living: “5 Essentials” of Chiropractic Marketing Propaganda
What do vitalism, old school chiropractic subluxations, germ theory denial, detox supplements, marketing gimmicks, and practicing way beyond a reasonable scope have in common?

If you feel better, should you stop taking your antibiotics?
A recent paper suggests that patients would be better off stopping antibiotics when they feel better, instead of completing the entire amount prescribed. Could this approach reduce antibiotic overuse and the risk of widespread resistance?

IBM’s Watson versus cancer: Hype meets reality
Five years ago, IBM announced that its supercomputer Watson would revolutionize cancer treatment by using its artificial intelligence to digest and distill the thousands of oncology studies published every year plus patient-level data and expert recommendations into treatment recommendation. Last week, a report published by STAT News shows that, years later, IBM's hubris and hype have crashed into reality.

Another Child Harmed by Pseudomedicine: Lead Poisoning from a “Homeopathic Healing” Bracelet
The CDC has published a report on yet another child harmed by exposure to a caregiver's belief in quackery...and the toxic level of lead found in a "homeopathic" teething bracelet.
Is the use of “Open-Label” Placebo Ethical in the Treatment of Children?
Is the use of "open-label" placebo ethical in pediatric medical care, or any care for that matter? A recent article in Pediatrics discussing this issue comes to a flawed conclusion based on a misunderstanding of placebo and of the literature on placebo without deception.
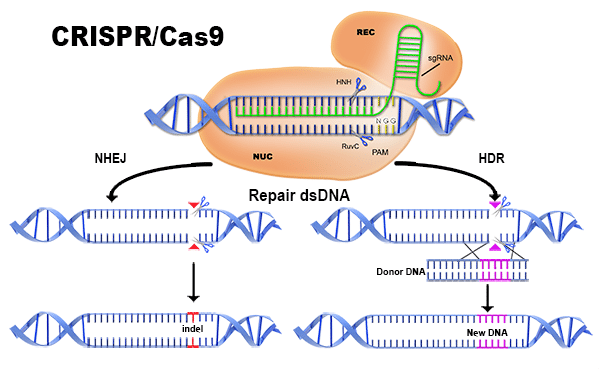
The Promise of CRISPR
CRISPR is the latest rock-star medical technology that promises to revolutionize medicine. Let's take a look at the hype and the reality.

Is something better than nothing? The many ineffective ways we treat nocturnal leg cramps
While leg cramps won't kill you, they can make you miserable when you are trying to sleep. There's not much evidence for effective treatments, and there are far more proposed treatments than there is evidence.
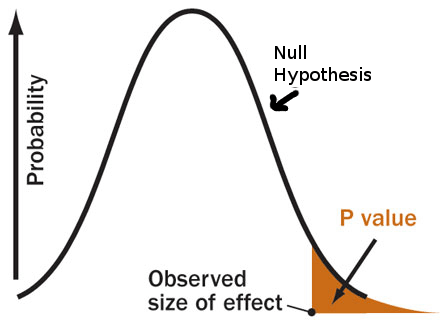
0.05 or 0.005? P-value Wars Continue
The p-value is under fire yet again, but this time with some quick-and-dirty solutions (and some long-and-onerous ones too) to the problems created by relying on this quick-and-dirty test.

Abraham Cherrix is alive and well because of science-based medicine
Although I haven't discussed it here in depth, the case of Abraham Cherrix is an instructive example. Eleven years ago, he and his parents chose quackery over science-based medicine to treat his cancer. He's alive now because he finally realized the error of his decision and underwent chemotherapy and a bone marrow transplant.