Category: Science and Medicine

Is there a reproducibility “crisis” in biomedical science? No, but there is a reproducibility problem
Reproducibility is the key to scientific advancement. It has been claimed that we suffer from a "reproducibility crisis," but in reality it is a chronic problem in reproducibility. Here we will look at the scope of the problem and strategies to address it.
Does your antivax doctor have another agenda?
Several weeks back, I wrote a piece in praise of Michigan’s Fresh Air Camp’s decision to admit only properly vaccinated children. Predictably, there was a bit of a backlash from people who, despite the obvious benefits, oppose vaccinations. I can’t fault a parent for the decisions they make for their kids. We all work from the gut when it comes to our...
Newborn Phototherapy and Cancer: Cutting Edge Research or “Big Data” Failure?
While social media and news outlets were reacting, or in some cases overreacting, to a new rodent-based medical study on the unlikely link between cell phone use and brain cancer last month, two studies and an accompanying commentary were quietly published in Pediatrics that raised similar concerns. Rather than cell phone use, the proposed potential cause of pediatric cancer in these newly...
Fooling Myself
The first principle is that you must not fool yourself — and you are the easiest person to fool. –Richard Feynman I like to think of myself as a rational person, but I’ve been fooled by my own experience again and again. I’ve made bad decisions and wasted time and money believing what I was seeing, instead of being objective and looking...
Uncertainty in Medicine
Medicine is an uncertain business. It is an applied science, applying the results of basic science knowledge and clinical studies to patients who are individuals with differing heredity, environment, and history. It is commonly assumed that modern science-based doctors know what they are doing, but quite often they don’t know for certain. Different doctors interpret the same evidence differently; there is uncertainty...
Australian Chiropractor Ian Rossborough Promises to Stop Treating Children…for Twenty Days
Before I begin this brief update to my recent post on Australian baby chiropractor Ian Rossborough’s “crack heard round the world,” I want to give a quick thanks to Jann Bellamy for organizing our day of Science-Based Medicine at NECSS last week. It was an amazing experience sharing the stage with the SBM crew for my first public presentation, and finally getting...
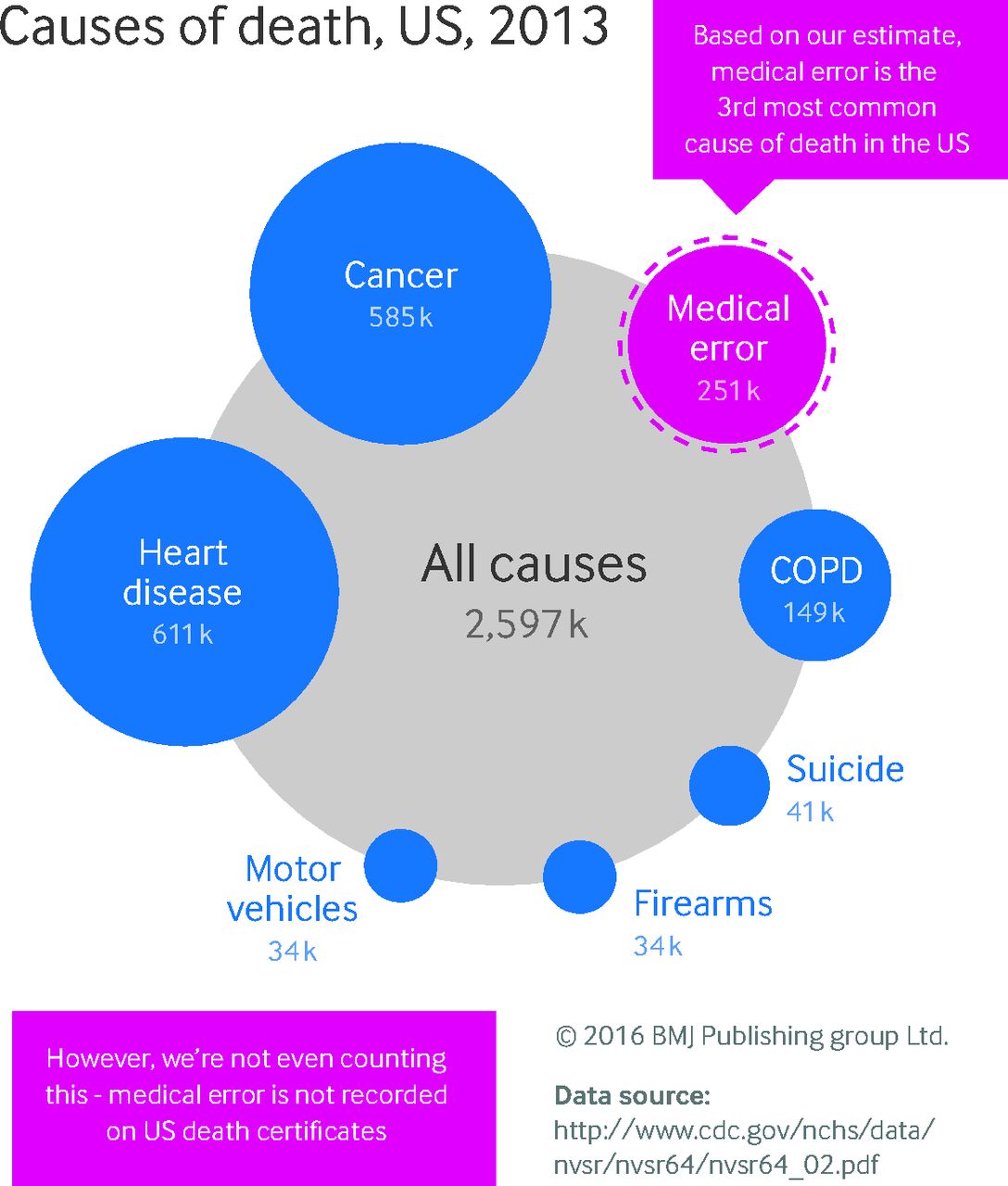
Are medical errors really the third most common cause of death in the U.S.?
A regurgitation of existing data suggested that medical error is the third leading cause of death in America. Is it true? Spoiler alert! No. No it's not. While medical error can and should be reduced, this BMJ article does not justify claims that doctors are a leading cause of death in the United States.

The Crack Heard Round the World
In January, Melbourne chiropractor Ian Rossborough uploaded a video to YouTube of himself treating a 4-day-old premature infant. The video, one of many that can be found on his “Chiropractic Excellence” channel, is for educational purposes only, intended to teach the world about the miraculous benefits of chiropractic care for a wide variety of conditions. Although the cynical among us may proclaim...
Is there a naturopathic standard of care?
Public outcry over the death of Ezekiel Stephan, the 19-month-old Alberta toddler who died of bacterial meningitis in 2012, continues to grow following last’s weeks court decision, which found both of his parents guilty of failing to provide the necessaries of life. David and Collet Stephan failed to seek appropriate medical care for their obviously-ill child, instead relying on a variety of...
Separating Fact from Fiction in the Not-So-Normal Newborn Nursery: Chiropractic and Brachial Plexus Injury
Thanks to a hot tip from a follower on Twitter, I’ve once again found myself neck deep in chiropractic propaganda involving the care of a pediatric patient. The case as presented involves, among numerous specious assumptions, claims of successfully treating an infant’s paralyzed arm using chiropractic philosophy and spinal adjustment techniques. As I will explain in detail, this “miracle” is just another...

