Category: Science and the Media
Why Are Sensible Medicine Doctors Indifferent to the Nonsense Comments of Sensible Medicine Commentators? As Instructed, I Consider the Dualities of Interest and Motivating Biases.
Sensible Medicine doctors often utter the words "do an RCT". So why are their readers so ignorant about RCTs?

Dr. Adam Cifu: “We Now Need to Accept That This is Here to Get Infected With Again and Again.”
If Dr. Adam Cifu were genuinely concerned about vaccine hesitancy, I would strongly encourage him to learn about the anti-vaccine movement. He'll discover that it is fueled not by a lack of "robust data" on COVID boosters, but rather by exactly the sort of mistrust and anti-vaccine misinformation spread by his own blog and collaborators.
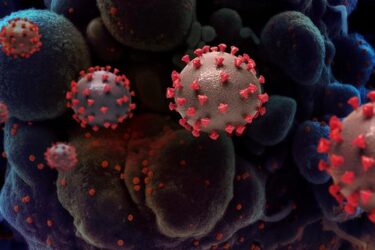
Hospital Measures Prevented COVID Transmission
A new study finds that hospital measures to limit the spread of COVID-19 worked, and we probably should keep them.

Dr. Lucy McBride: “As physicians, dispensing false hope is dangerous & unethical.”
The many sheltered physicians like Dr. Lucy McBride who confidently said herd immunity was at hand and fear of COVID was pathological are the last people who should be sanctimoniously sermonizing about the importance of trust in medicine.
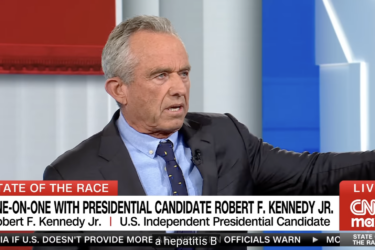
RFK Jr. and his “I’m not anti-vaccine” rejoinder to being confronted with his past antivax statements: A primer
On Friday, CNN host Kasie Hunt interviewed antivax presidential candidate Robert F. Kennedy, Jr. Although she did better than most journalists confronting him for his past antivax statements in that she played a clip of one of his antivax statements, she clearly hadn't anticipated his response, which should have been very predictable given that he's been using it for at least 15...

When a “gender critical” is a runner-up for the Maddox Prize for standing up for science…
Helen Joyce, a virulently anti-trans "gender critical" campaigner, was recently shortlisted for the Maddox Prize, which purports to recognize people who "who stand up for science and evidence, advancing public discussion around difficult topics despite challenges or hostility," even though she promotes an agenda that denies science and demonizes trans people. How could this have happened?

Misinformation is pervasive, and AI will turbocharge it
Is it possible to refute an infinite amount of AI-generated health misinformation?

Trust in science and vaccines continues to decline. Why?
Recent evidence shows that public trust in science and vaccines has declined markedly since the pandemic. Why is this, and is there anything we can do about it?

Robert F. Kennedy Jr. comes home to his antivax roots…again
Robert F. Kennedy Jr. gave the keynote speech at the second annual meeting of his antivax organization, Children's Health Defense. Once again, he demonstrated that not only is he still antivax as hell, but that his proposals are even more bizarre than before. Truly, it was a homecoming for him.


