Category: Surgical Procedures

First Whole Eye Transplant
A whole eye transplant did not restore vision, but is still an important advance.

The Facemaker
Lindsey Fitzharris' book describes the amazing innovations in plastic surgery brought about because of the horrors of World War I.

Gender-Affirming Care is Not Experimental, Part II
A lot of the "facts" about providing healthcare to transgender youth turn out to be not actually facts. We present here a summary of the evidence relating to transition-related health care for transgender adolescents.

Legislative alchemy and abortion: How the fall of Roe v. Wade will degrade science-based medicine
The U.S. Supreme Court overturned Roe v. Wade on Friday, eliminating the federal right to an abortion. What does that mean for science-based reproductive health and science-based medicine in general? Hint: It's not good, even for areas of medicine outside of reproductive health.
Breakthrough Heart Xenotransplantion from Pig
In a first, a bioengineered pig heart is transplanted into a human donor, indicating we are on the threshold of a game-changing option for organ transplantation.
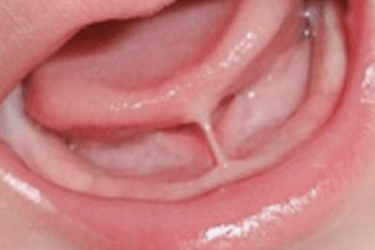
The Frenetic Frenum Freeing Frenzy
What problems do tongue-ties cause? Do all of them need to be clipped?
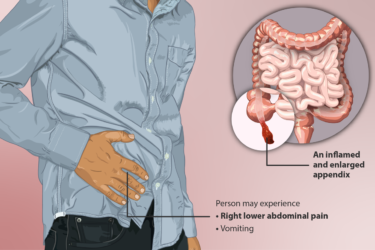
Appendicitis: Surgical vs. Medical Treatment
Surgery or antibiotics for appendicitis? This new study can help with the decision.
When Doctors Refuse to Believe Evidence
Paul Offit's new book covers the evidence for many surgeries, medications, and screening tests that have been proven ineffective and harmful yet are still being used by doctors who refuse to follow the science.
Ian Harris on “Surgery, the Ultimate Placebo”
Ian Harris explains that more than half of commonly performed surgical operations may be placebos. Adequate studies using a blinded control group are essential.